Urine Calcium (Ca), (Quantitative 24 hrs urine calcium)
Urine Calcium (Ca)
Sample for Urine Calcium (Ca)
- 24 hours of urine is collected in the acid wash bottle.
- Add 10 to 20 mL of 6M/L HCl.
- 1 to 2 mL of a random urine sample can also be evaluated.
- Refrigerate the urine during collection.
- Or acidify the urine to pH <2.0 to dissolve the calcium salts.
Precautions for Urine Calcium (Ca)
- Wash the bottle with dilute HCl and then rinse with water.
- Avoid contamination with calcium.
- Don’t use cork because it may contaminate the urine.
- If this test is done for metabolic disorders, advise the patient to have a low-calcium diet and stop calcium medications 1 to 3 days before the urine collection.
- For patients with renal stones, the formation should have the same routine diet for the last three days before collecting the urine. Can continue medications.
Indications for Urine Calcium (Ca)
- This is done to evaluate calcium intake (hypercalcemia).
- This also tells the rate of :
- Absorption of calcium from the GI tract.
- Bone Resorption.
- Renal loss.
- Measurement of calcium levels in urine and serum levels is used to diagnose and monitor calcium metabolism disorders.
- This test is also used in the stone evaluation and follow-up.
- Urine calcium is also advised for the calcium intake or rate of intestinal absorption, bone resorption, and renal loss.
Pathophysiology of Calcium (Ca)
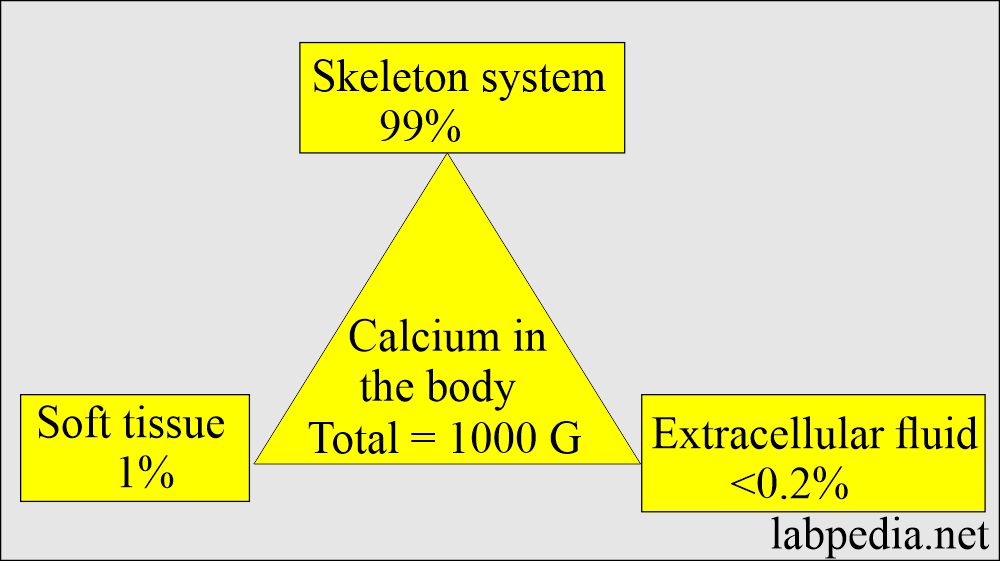
- Calcium is the fifth most common element in the body.
- The average human body contains 1 kg of calcium.
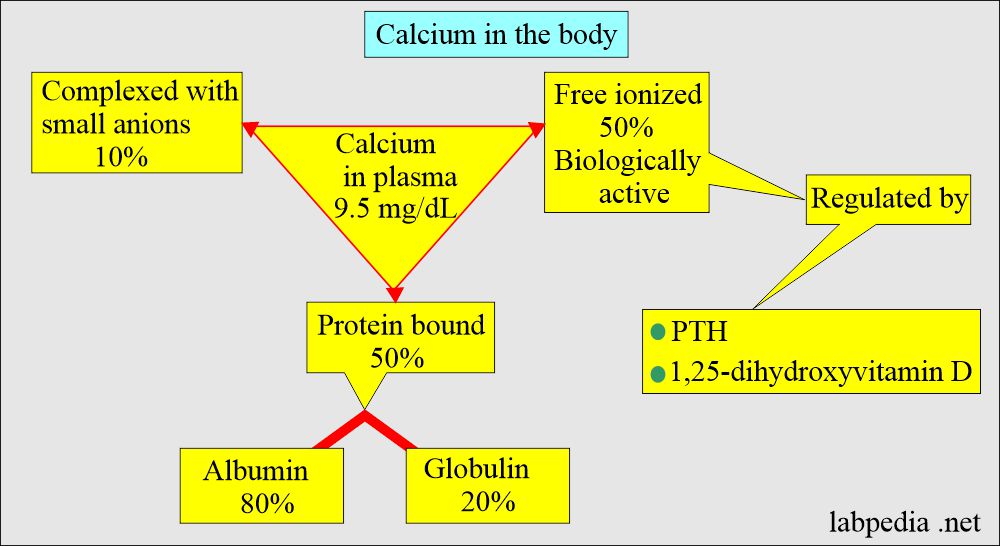
- Calcium exists in three forms in the blood.
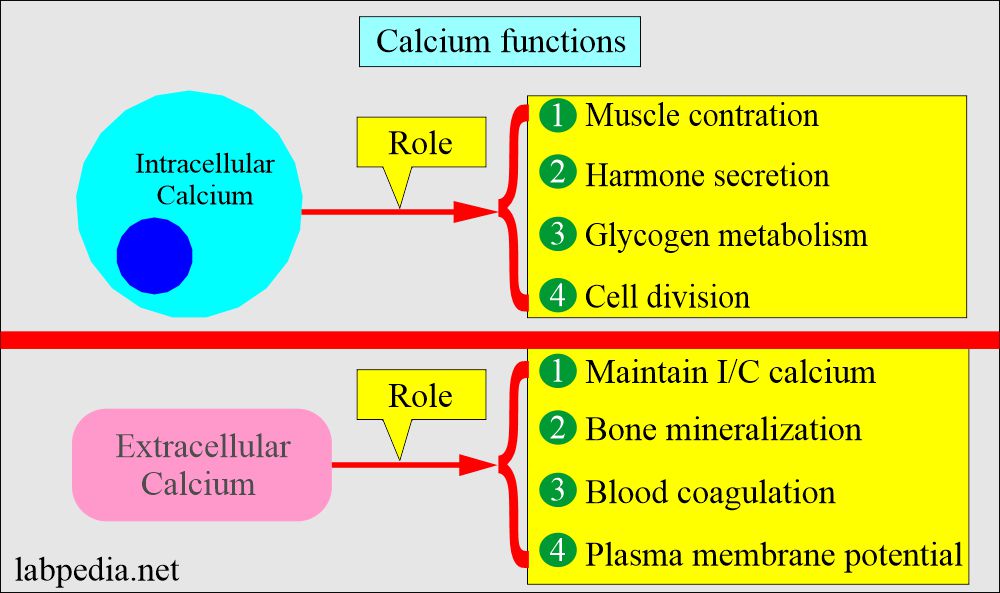
- Calcium in the body exists as intracellular and extracellular, and both have different functions.
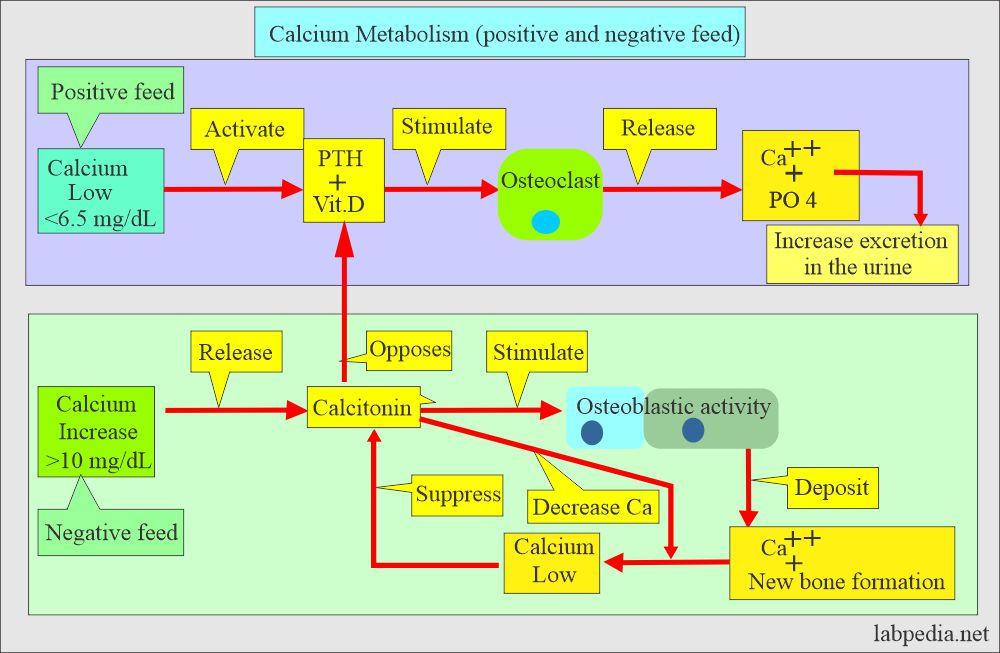
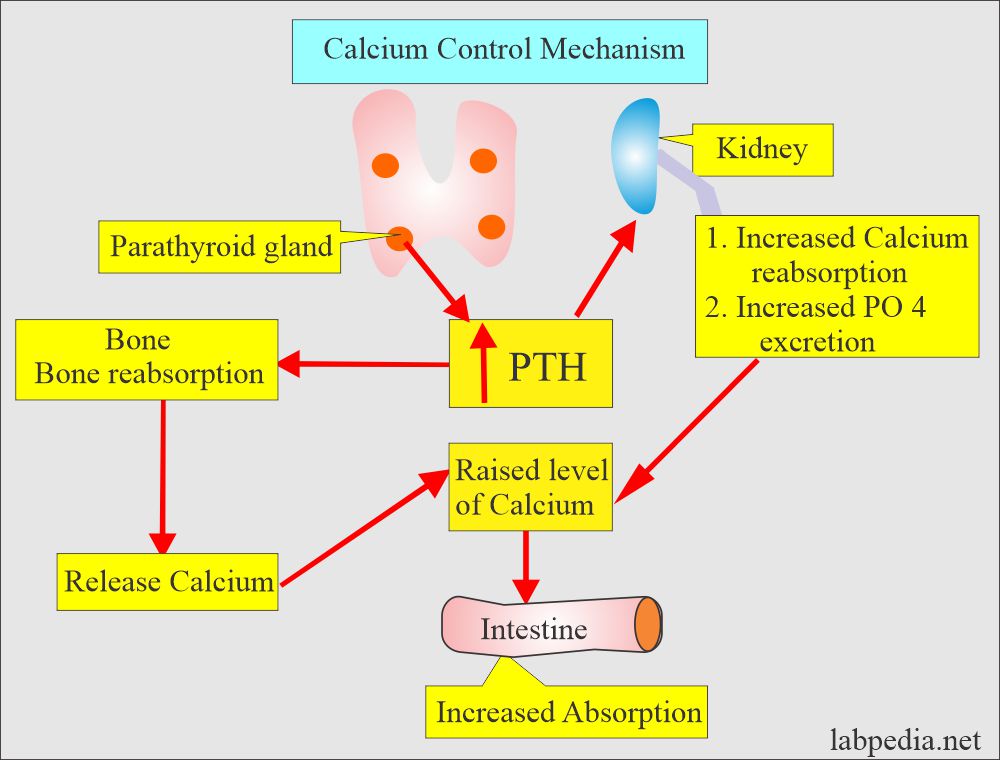
- The parathyroid hormone maintains blood calcium levels.
- PTH indirectly increases the absorption of calcium from the gastrointestinal tract by producing the vit. D.
- PTH increases the serum calcium level by increasing bone resorption and mobilizing Calcium.
- Urine calcium is high in 30% to 80% of primary hyperparathyroidism cases, but it does not diagnostic.
Calcium excretion:
- Mostly calcium is lost in the stool.
- A minimal amount is excreted in the urine.
- In hypercalcemia, there is increased secretion of calcium in the urine.
- In hypocalcemia, there is decreased secretion of calcium in the urine.
- Urinary calcium excretion is dependent upon the dietary intake of calcium.
Increased urinary calcium takes place due to the following:
- Increased intestinal calcium absorption.
- The defect in the renal tubular reabsorption.
- Loss or reabsorption from the bone.
- Or a combination of the above possibilities.
- In primary hyperparathyroid disease, 30 to 80 % of the patient has high urinary calcium.
- Urine calcium does not have much value in the differential diagnosis.
Normal urinary calcium
Source 1
| Diet | mg/day | mmol/Kg/day |
| Infants and child |
up to 6.0 mg/Kg/day |
0.15 |
| Ca-free diet | 5 to 40 | 0.13 to 1.0 |
| Low to average Ca-diet | 50 to 150 | 1.25 to 3.75 |
| Average Ca-diet | 100 to 300 | 2.50 to 7.50 |
- The average Calcium diet is 800 mg/day.
Source 4
- Normal diet = 100 to 300 mg/ 24 hours or 2.50 to 7.50 mmol/day.
- Low calcium diet = 100 to 150 mg /24 hours or 1.25 to 3.75 mmol/day.
Another source
- 50 to 250 mg/24 hours.
False raised values are seen in the following:
- Some of the drugs like calcitonin, vitamins A, K, and C.
- Corticosteroids.
- Urine is taken after meals with a high calcium intake, e.g., milk.
- Increased exposure to sunlight.
- Immobilization, especially in children.
False decreased values are seen in the following:
- Increased ingestion of PO4, HCO3–, and antacid.
- Thiazide diuretics.
- Lithium therapy.
- Alkaline urine.
- Oral contraceptives and estrogens.
Increased urinary calcium:
- In hyperparathyroidism, 30 to 80% of the cases.
- Paget’s diseases.
- Renal diseases.
- Sarcoidosis.
- Breast cancer.
- Urinary bladder cancers.
- Multiple Myeloma.
- Bone metastasis (osteolytic).
- Vit.D intoxication.
- Thyrotoxicosis.
- Osteoporosis.
- Fanconi’s syndrome.
- Idiopathic hypercalciuria.
- Prolonged immobilization.
Decreased urinary calcium:
- Renal osteodystrophy.
- Rickets
- Hypoparathyroidism.
- Pre-eclampsia.
- Vit.D deficiency.
- Metastatic carcinoma of the prostate.
- Preeclampsia.
- Acute renal failure, nephritis, and nephrosis.
- Malabsorption conditions like :
- Celiac disease.
- Sprue disease.
- Steatorrhea.
Questions and answers:
Question 1: How much body contains calcium?
Question 2: What is the role of calcitonin in our body?
Drugs like Thiazide and oral contraceptives leads to decrease level.