Tumor Marker:- Part 10 – Thyroglobulin (Tg) as Tumor marker
Thyroglobulin (Tg)
Sample for Thyroglobulin (Tg)
- Venous blood is needed to prepare the serum.
Purpose of the test (Indications) for Thyroglobulin (Tg)
- Thyroglobulin is advised after the treatment of thyroid cancer.
- This is done to diagnose hyperthyroidism.
- This is the tumor marker for well-differentiated thyroid cancer (follicular and papillary).
- Thyroglobulin is not elaborated by medullary or anaplastic thyroid cancer.
- This can also help to monitor thyroid cancer or metastatic cancer.
Precautions for Thyroglobulin (Tg)
- Make sure that patients are off the thyroid medication for 6 weeks.
- Evaluate the TSH level before testing the Tg.
- Anti-Tg antibodies are present in 15 to 35% of patients with thyroid cancer. These will interfere with the Tg results.
Pathophysiology of Thyroglobulin (Tg)
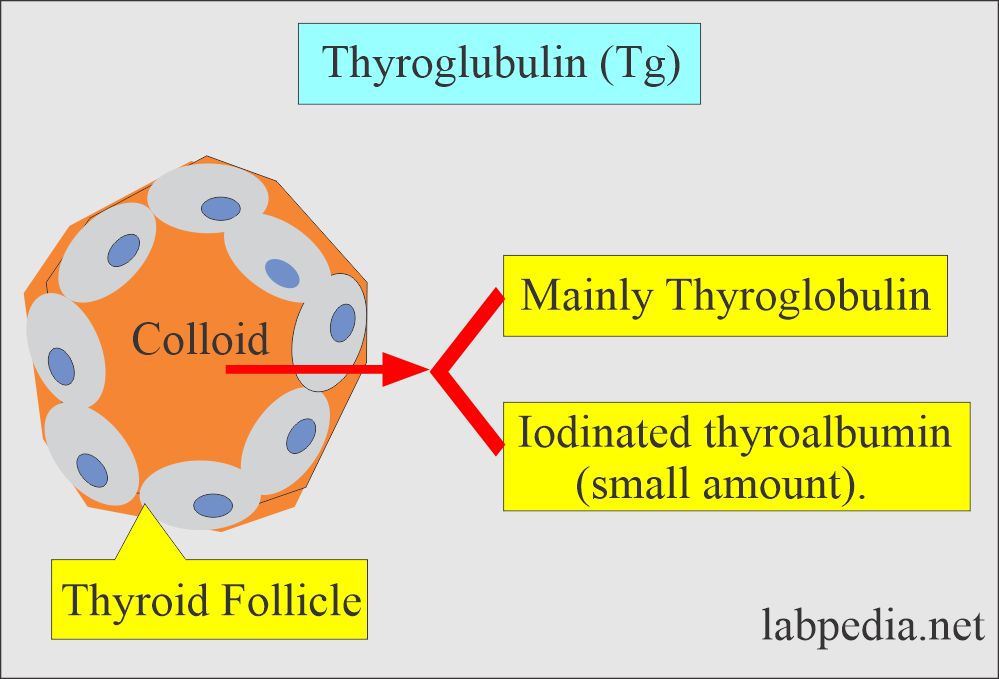
- Thyroglobulin is a glycoprotein, 660kD, and iodinated secretion of epithelial cells of the thyroid gland.
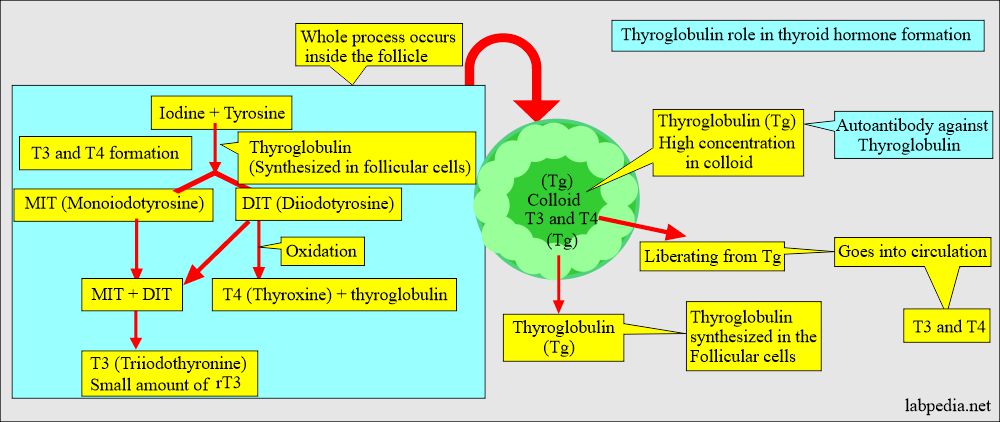
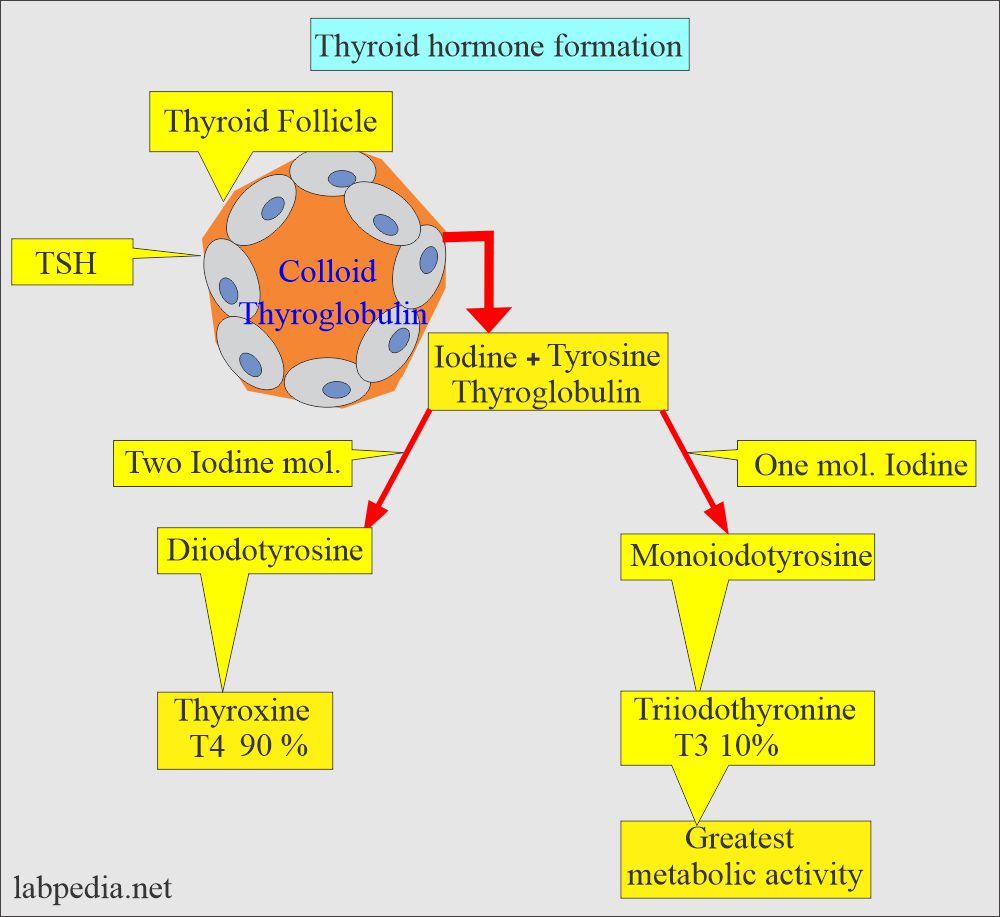
- It is synthesized and secreted by the thyroid follicular cells.
- Thyroglobulin is a precursor of the thyroid hormone.
- This may be made by normal epithelial cells as well as by cancer cells.
- Raised values of thyroglobulin (Tg) are found in the following:
- Thyrotoxicosis.
- Thyroiditis.
- Iodine deficiency.
- Benign thyroid adenomas.
- Differentiated thyroid carcinomas (follicular and papillary carcinoma and papillary-follicular carcinoma).
- Medullary carcinoma does not produce thyroglobulin (Tg).
- If there is a very low level of Tg after the surgery of the thyroid indicates very little leftover in the thyroid tissues.
- The iodinated secretion also contains T3, T4, and hormones.
Thyroglobulin (Tg) is also called a tumor marker.
- Half-life is about 65 hours (another reference days 8 to 22 hours).
- It takes nearly a month before thyroglobulin becomes undetectable following total thyroidectomy.
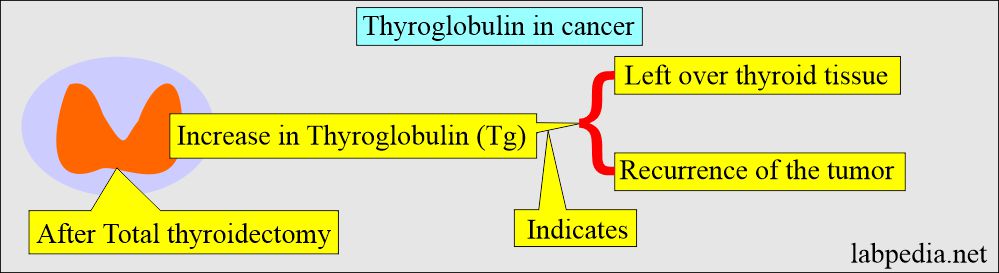
- In the operated cases of cancer, Thyroglobulin (Tg) postoperatively gives the idea about the activity of the disease and the volume of thyroid tissue left behind.
- The rising level of Thyroglobulin (Tg) indicates tumor recurrence and progression.
- Thyroglobulin (Tg) is also raised in benign conditions as well, so not specific or sensitive for the diagnosis of thyroid cancer.
- After thyroidectomy, thyroid hormone replacement is needed for normal body metabolism.
- Because of thyroid hormone replacement, TSH level is low, so there is minimal stimulation of thyroid cells.
- To stimulate Thyroglobulin (Tg) in thyroid cancer cases after thyroidectomy, stop the hormone replacement for at least 6 weeks.
- Now TSH will be stimulated, stimulating Thyroglobulin (Tg) production from the epithelial cells.
- If there are any leftover thyroid cancer cells, the Thyroglobulin (Tg) level will increase.
- After surgery and radiation in cancer patients, the Thyroglobulin (Tg) level is undetectable.
Advantages of thyroglobulin in cancer patients:
- A thyroid tumor scan with I131 is required to differentiate begin and cancer cells.
- Thyroglobulin estimation advantage is less exposure to radiation in the form of I131.
- With thyroglobulin estimation, I131 is not needed.
- Patients with metastasis are not detected by the I131 scan, where thyroglobulin (Tg) is raised.
Thyrogen-stimulation test.
- Thyrogen is a synthetic purified recombinant source like a human thyroid-stimulating hormone (TSH).
- Thyrogen is synthetic TSH and is called thyrotropin alpha.
- Keep the patient off the hormone replacement therapy.
- Thyrogen two injections are given on two consecutive days.
- Take a blood sample of the patient for thyroid hormones and thyroglobulin.
- Normal thyroid tissue and thyroid cancer cells raise >10 times Tg level by TSH stimulation.
- Thyrogen stimulates the thyroid gland and raises the thyroglobulin (Tg) level.
- Advantages of thyrogen test:
- It monitors patients who have undergone thyroid surgery.
- It can detect residual tumors.
- It helps to determine the proper dosage of hormone replacement therapy.
Presence of antithyroglobulin antibodies:
- Anti-thyroglobulin antibodies are present in 10% of the normal population and 20% of those with thyroid cancer and are a major issue in thyroglobulin testing.
Normal Thyroglobulin (Tg)
Source 1
| Age | ng/mL |
| Cord blood | 24.4 ± 3.7 |
| One hour | 29.7 ± 4.2 |
| 48 hours | 41.9 ± 5.8 |
| Adult | 3 to 42 |
| Thyroid patient | <5 |
- To convert into SI unit x 1.0 = µg/L
Male Thyroglobulin (Tg)
- 0 to 11 months = 0.6 to 5.5 ng/mL.
- 1 to 11 years = 0.6 to 50.1 ng/mL.
- Adult = 0.5 to 53 ng/mL.
Female Thyroglobulin (Tg)
- 1 to 11 months = 0.5 to 5.5 ng/mL.
- 1 to 11 years = 0.5 to 52.1 ng/mL.
- Adult = 0.5 to 43 ng/mL.
- Another source gives normal values as follows:
- Adult = 3 to 42 ng/mL.
- Newborn = 36 to 48 ng/mL.
- 87% of normal adults have a serum value of <10 ng/mL.
Increased Thyroglobulin (Tg) level is seen in:
- Thyroid follicular and papillary carcinoma.
- Thyroid adenoma.
- Untreated and metastatic thyroid cancer.
- Subacute thyroiditis, Hashimoto’s thyroiditis, and Grave’s disease.
- Benign thyroid adenoma.
- Hypothyroidism.
- Recurrence of the metastatic tumor after the treatment.
Decreased Thyroglobulin (Tg) level is seen in:
- Infants with goiter (Hypothyroidism).
- Thyrotoxicosis factitia.
Questions and answers:
Question 1: What is thyrogen test?
Question 2: What is the site of formation of thyroglobulin?