Prothrombin Time (PT)
Prothrombin Time (PT)
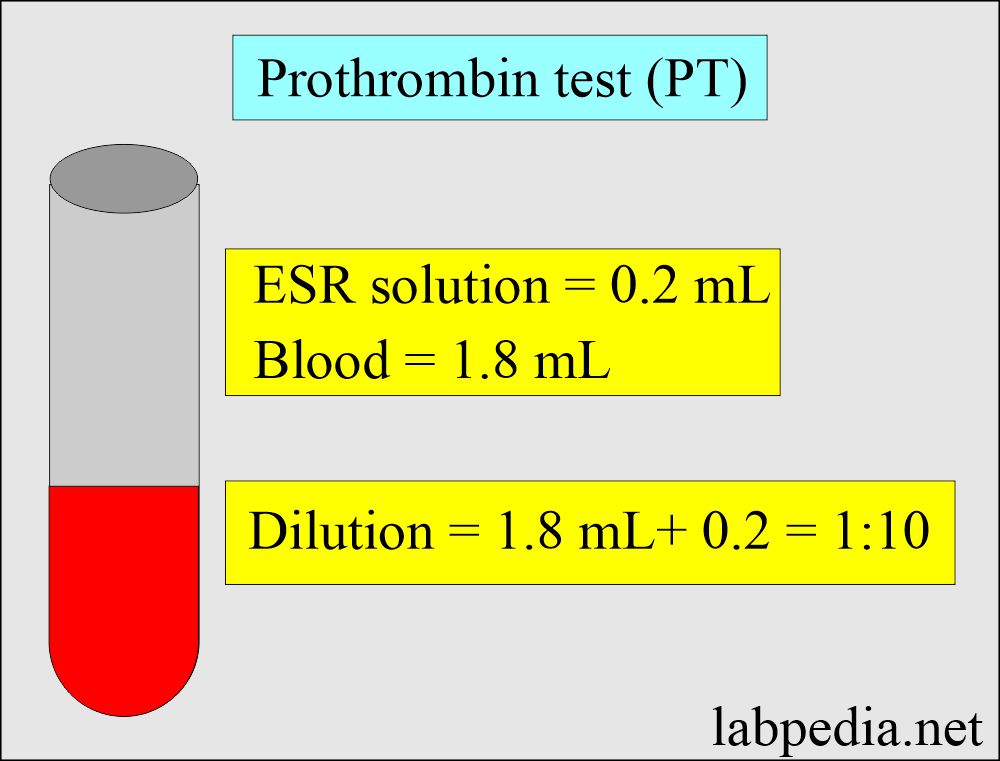
Sample for Prothrombin Time (PT)
- The blood sample is taken with ESR (sodium citrate) solution.
- The blood sample is 1.8 ml, and the ESR solution is 0.2 ml.
Precautions for Prothrombin Time (PT)
- Alcohol intake can increase PT time.
- A high-fat diet may decrease PT time.
- Some drugs decrease PT, like anabolic steroids, digitalis, Benadryl, griseofulvin, oral contraceptives, vitamin K, and chloral hydrate.
- Some drugs can increase PT, like aminosalicylic acid, barbiturates, beta-lactam antibiotics, chloramphenicol, clofibrate, heparin, methyldopa, neomycin, quinidine, quinine, sulphonamides, and salicylates.
Indications for Prothrombin Time (PT)
- This is one of the screening tests for coagulation.
- This test evaluates the extrinsic pathway defect.
- This test also finds a common pathway defect.
- This test is done For the screening of prothrombin deficiency.
- PT is also used to evaluate dysfibrinogenemia.
- PT is done to monitor the heparin and coumarin effect.
- In the case of bruises and abnormal bleeding.
- In the case of Vit. K deficiency.
- This is advised as a liver function test.
- This is used to assess synthetic liver function.
- To monitor the Warfarin therapy.
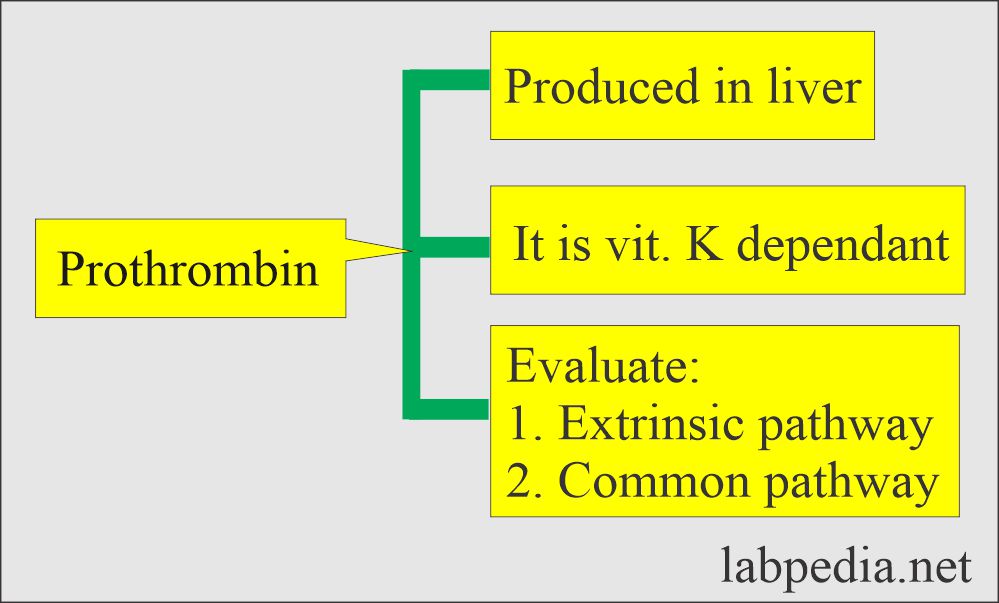
Pathophysiology of Prothrombin Time (PT)
- Prothrombin is a protein produced by the liver. Its molecular weight is 71,600 Daltons.
- Prothrombin helps in the clotting mechanism.
- Prothrombin production depends upon the adequate intake amount of Vit. K and its absorption.
- It is the most abundant and has a long half-life of the vit. K dependant clotting proteins circulate as a zymogen to serine protease.
- On clotting, prothrombin is converted into thrombin.
- Prothrombin
 Thrombin.
Thrombin.
- Prothrombin
- Factor II, VII, IX, and X depend upon the Vit. K for biosynthesis.
Prothrombin facts:
- The abnormality in prolonged Prothrombin test (PT):
- Factors I, II, VII, and X deficiency.
- Warfarin, liver diseases, and it. K deficiency.
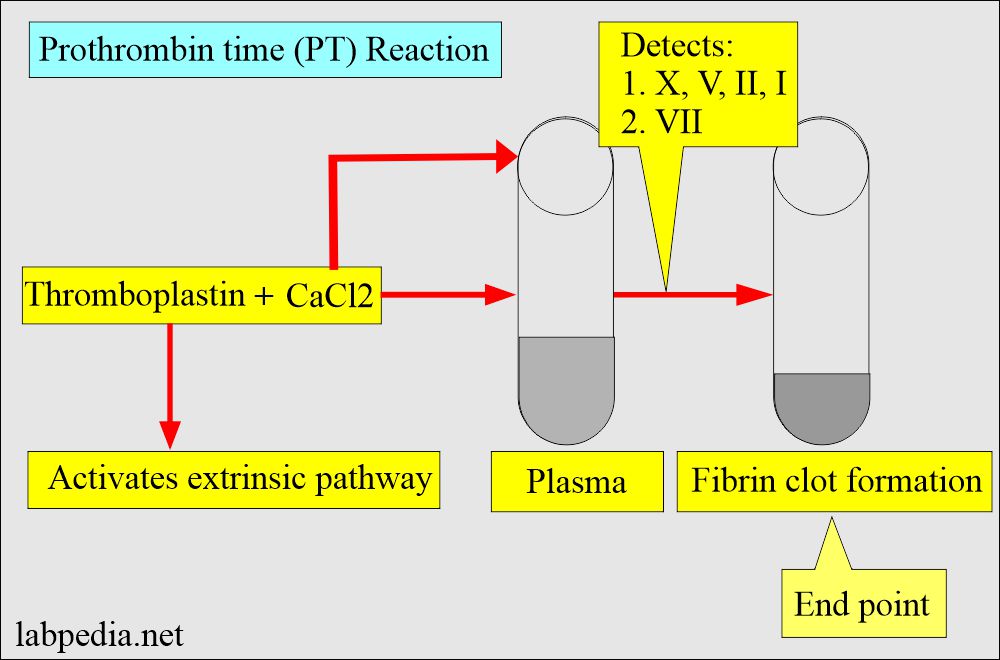
- Prothrombin Time (PT) measures :
- Extrinsic pathway (Activated VIIa)
- Tissue factor.
- Common pathways ( factor X, V, II, and fibrinogen ).
Principle of prothrombin time (PT):
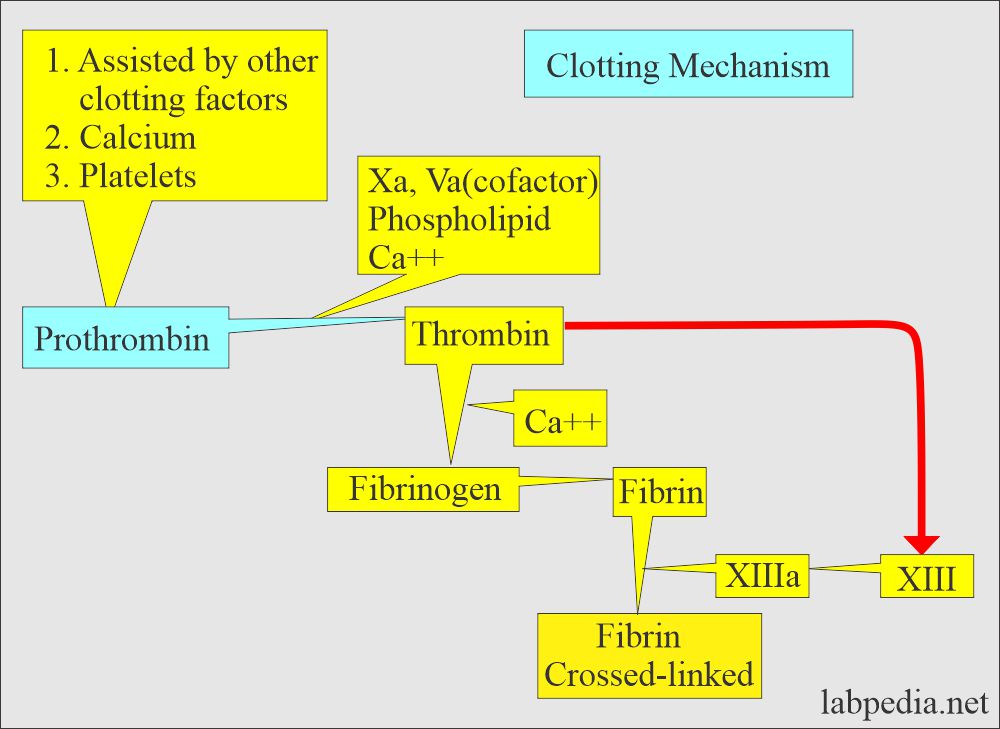
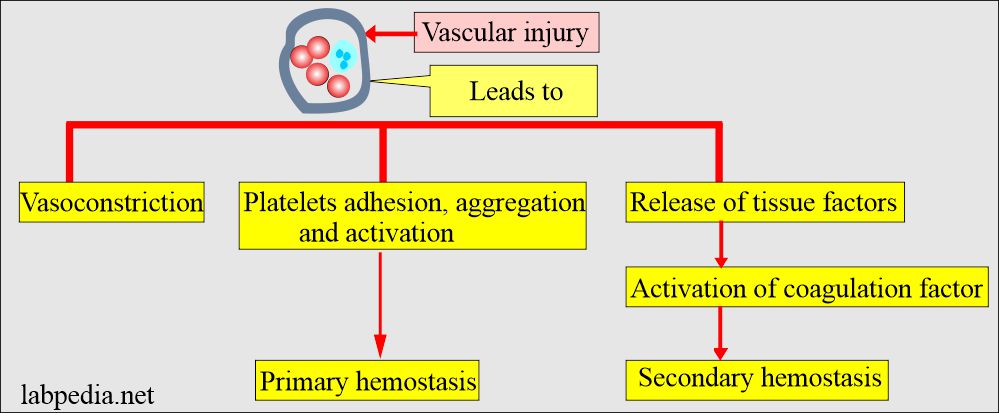
Clotting Mechanism
- The first stage is an aggregation of platelets to plug the damaged blood vessels.
- The second stage is by activation of clotting factors.
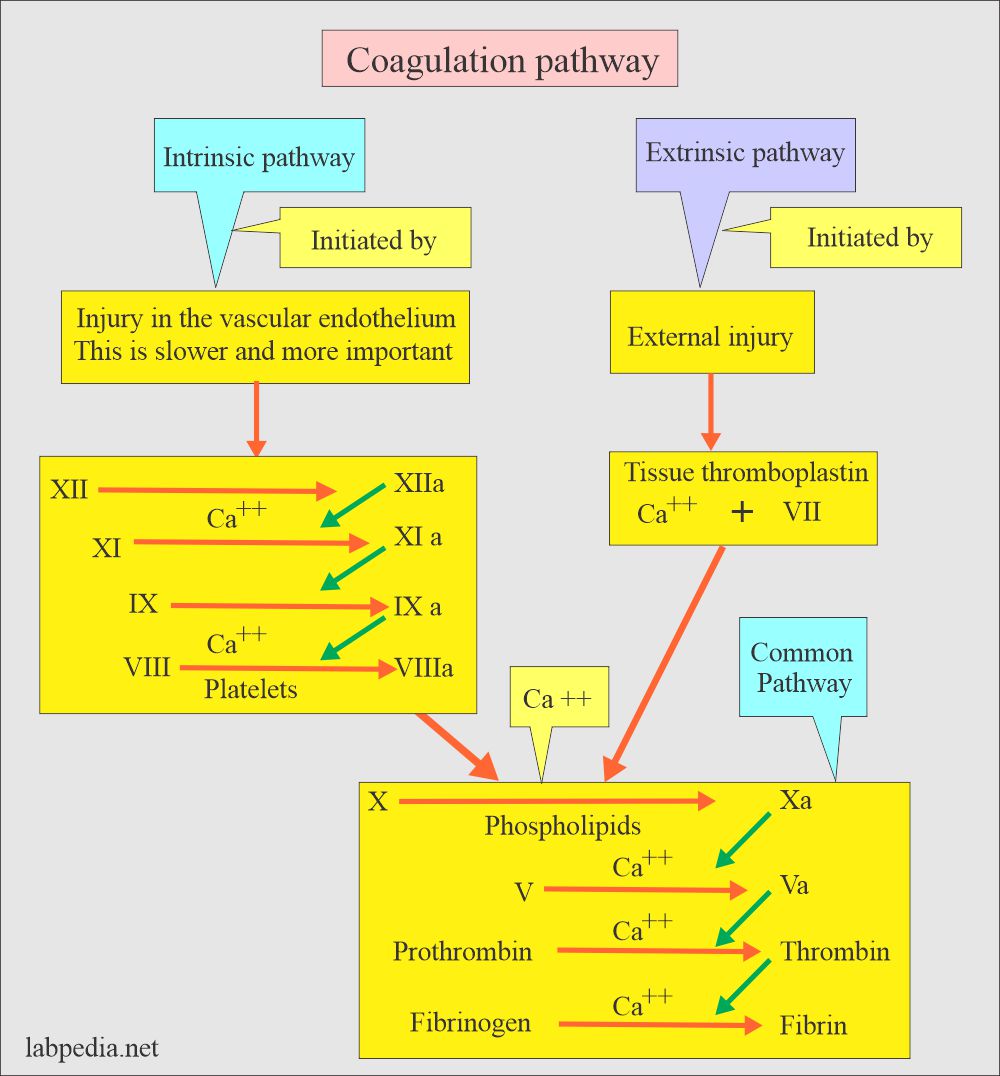
- The first phase of the activation of the intrinsic pathway.
- At the same time, the extrinsic pathway is activated.
- By common pathway, factor X is activated by the proteases formed by the intrinsic and extrinsic pathways.
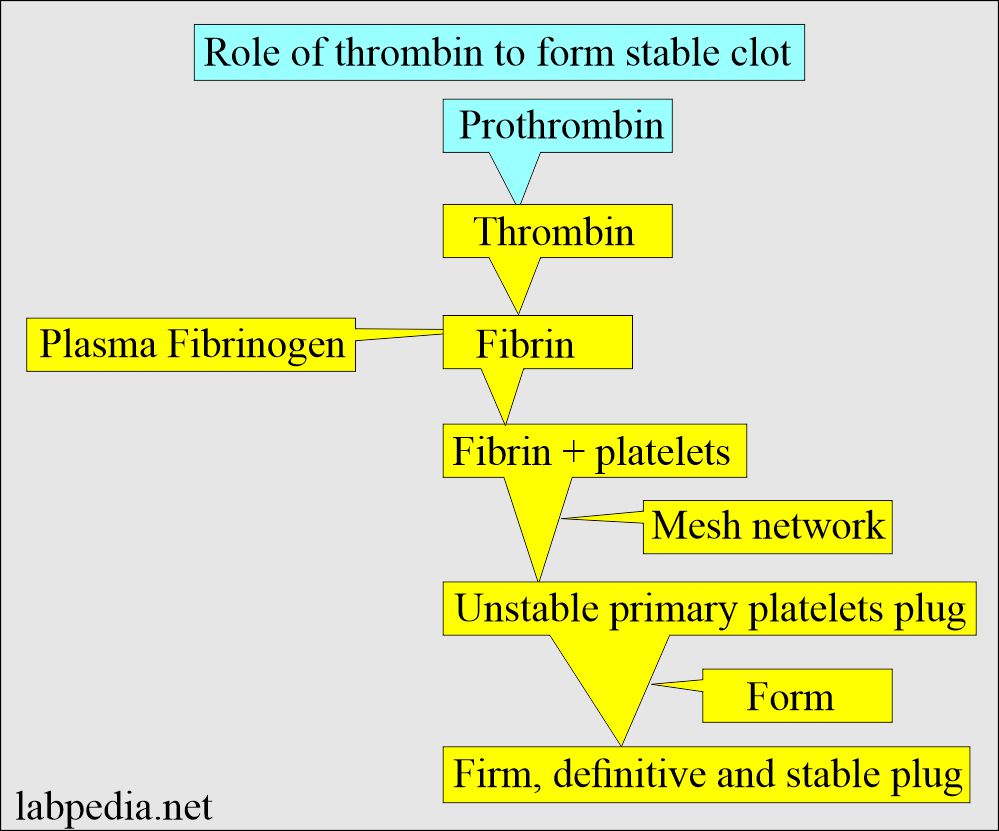
- The fourth phase is the conversion of prothrombin to thrombin in the presence of Factor X, Factor V, phospholipids, and calcium.
- Thrombin converts fibrinogen to fibrin.
- Fibrin is converted into a stable gel.
- XIII cross-links the fibrin and forms the clot.
NORMAL Prothrombin Time (PT)
- PT = 11 to 13 seconds (normally PT is 85% to 100%)
- (This may vary from lab to lab).
- This should be compared with the control, which will be around 11 to 14 seconds.
- Anticoagulant therapy response = 1.5 to 2 times the control value.
- Critical value = >20 seconds
- INR is an international normalized ratio. = 0.8 to 1.1
Increased Prothrombin Time (PT) is seen in the following:
- Deficiency of factor II (prothrombin), V, VII, and X.
- Liver diseases, like cirrhosis and hepatic failure.
- Factor I, II, V, VII, IX, and X are produced in the liver.
- This is abnormal when there is a severe disease of the liver.
- Biliary obstruction. There is a lack of bile which is needed for fat-soluble vitamins like Vit. A, D, E, and K for their absorption.
- Synthesis of factors II, VII, and X depends upon the vitamin K.
- Suppose the patients respond to Vit. K therapy in 1 to 3 days means no liver cell damage; rather, there is a biliary obstruction.
- If there is no response to Vit. k therapy, the patient has severe liver cell injury.
- Sprue, celiac disease, and chronic diarrhea.
- Vit. K deficiency, even in the newborn of the mother with Vit. K deficiency.
- Hemorrhagic disease of the newborn.
- Anticoagulant therapy (Warfarin and Coumadin).
- D I C.
- Factor 1 deficiency (Hypofibrinogenemia).
- Dysfibrinogenemia.
- Circulating anticoagulants are seen in lupus disease.
- Premature newborn.
- Salicylates intoxication.
- Massive blood transfusion.
Summary of Prothrombin Time (PT) and Partial thromboplastin time (PTT):
- Abnormal PTT alone
- Bleeding due to deficiency of factors V11, IX, and XI.
- Abnormal PT only
- Factor VII deficiency.
- Abnormal PT and PTT both
- Anticoagulant therapy.
- D I C.
- Vit. K deficiency.
- Liver diseases.
- Massive blood transfusion.
- Rarely due to Dysfibrinogenemia and deficiency of factors X, V, and II.
| Clinical condition | Prothrombin time | Thrombin time | APTT | Platelets count |
| Heparin therapy | prolonged mild | prolonged | prolonged | normal (the count is low) |
| Oral anticoagulants | Prolonged | normal | prolonged | normal |
| Circulating anticoagulant | normal/prolonged | normal | prolonged | normal |
| DIC | prolonged | prolonged | prolonged | low |
| Liver disease | prolonged | normal (rarely prolonged) | prolonged | low |
| Blood transfusion, massive | prolonged | normal | prolonged | low |
| Vit. K deficiency | prolonged | normal | prolonged | normal |
- Please, for more information, see PTT and APTT.
Questions and answers:
Question 1: What factor deficiency will be diagnosed by prothrombin time?
Question 2: What is the critical value of prothrombin time?