Malarial parasite:- Part 4 – Plasmodium Malariae, Benign Quartan Malaria
Plasmodium Malariae
Sample for Plasmodium Malariae
- Malarial parasites ( MP ) may be diagnosed from a patient’s blood smear with a fever.
- The best time to make a smear is during shivering.
- Make thick and thin blood smears.
- Serum needed for a Serological method and for PCR.
Definition of Plasmodium malariae
- Plasmodium malariae causes fever every 72 hours.
- It causes a fever every 72 hours.
- It infects older small RBCs.
Plasmodium Malariae facts
- This was recognized by the Greeks because of its fever presentation.
- This is a cosmopolitan parasite but not seen everywhere.
- 2% to 3% in Africa.
- Sporadic in Asia and S America.
- It is common in regions of tropical Africa.
- Also seen in India, Sri Lanka, Malaya, Java, New Guinea, and Europe.
- Sporadic in Asia and S America.
- Plasmodium malariae represents only a small percentage of infections.
Vector of Plasmodium malariae:
- These are seen in wild animals. Chimpanzees are also infected.
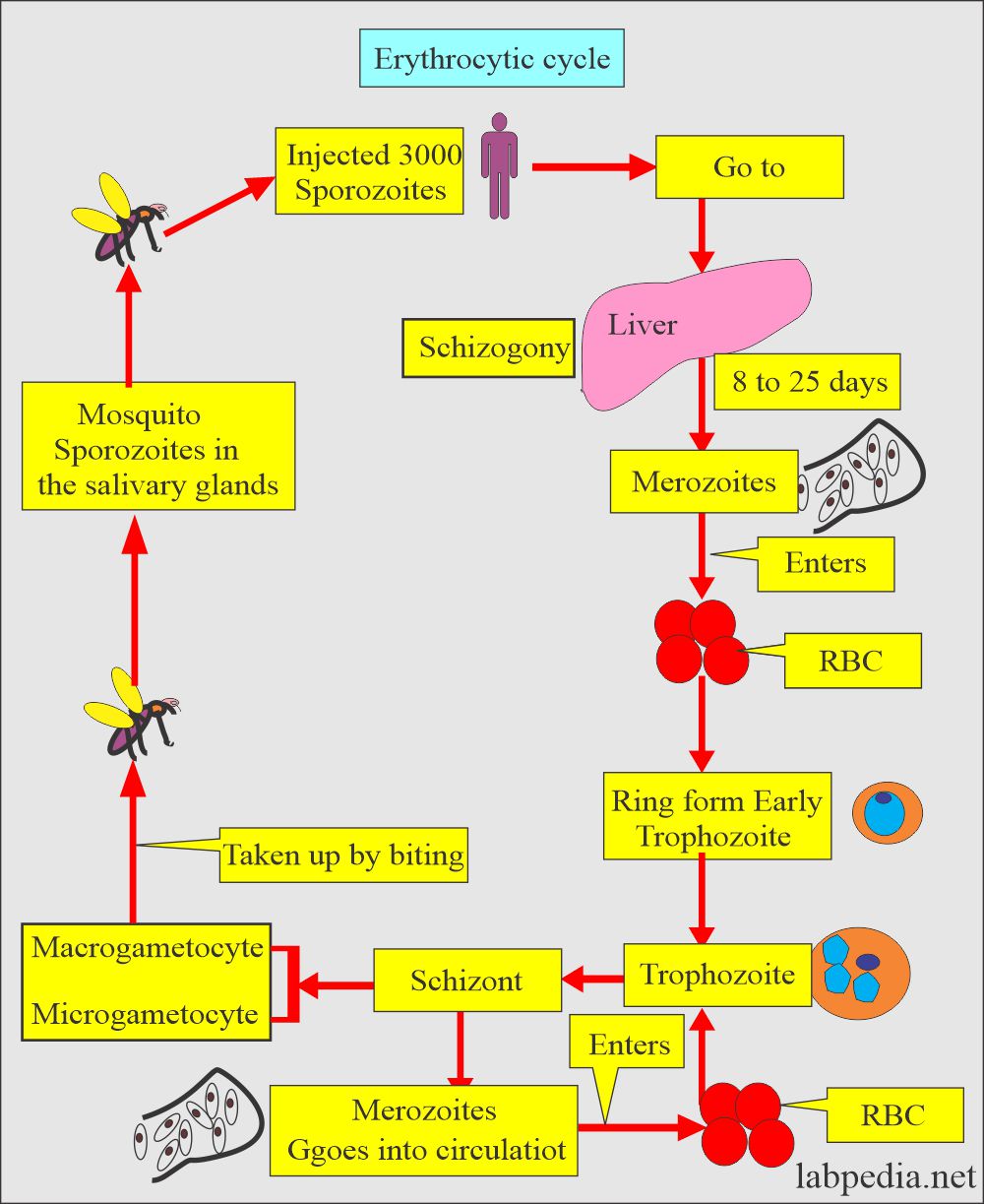
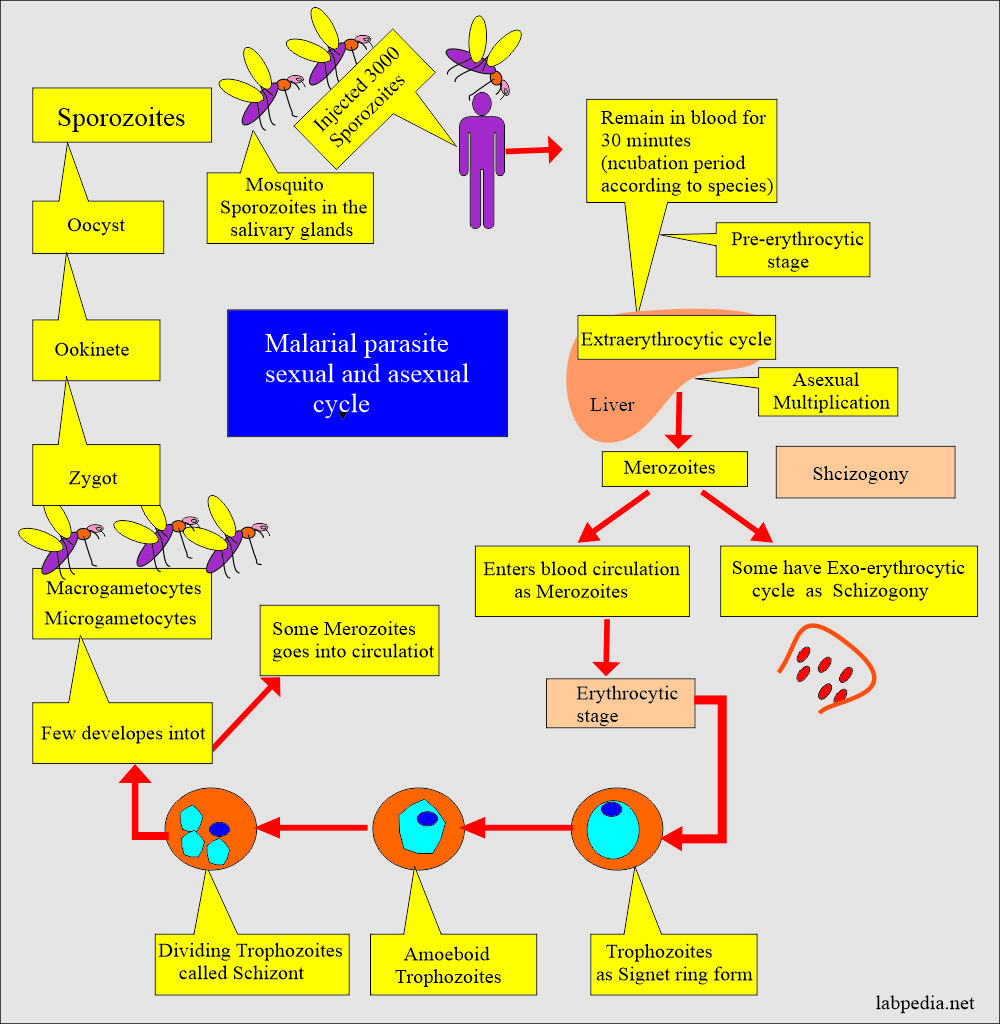
The exoerythrocytic cycle of Plasmodium Malariae
- It is completed in the liver in 13 to 16 days.
The erythrocytic cycle of Plasmodium Malariae
- Ring form typically occupies 1/6 of the infected RBC.
- It is smaller than P. vivax.
- There is a heavy chromatin dot.
- Pigments form early.
- Trophozoites are typically non-ameboid, with solid cytoplasm.
- The cytoplasm shows dark brown pigments that may mask the chromatin.
- Schizonts typically contain 6 to 12 merozoites.
- These are arranged in rosettes or in irregular clusters.
- Central brown-green pigment may often be visible.
- Parasite completely fills the RBC.
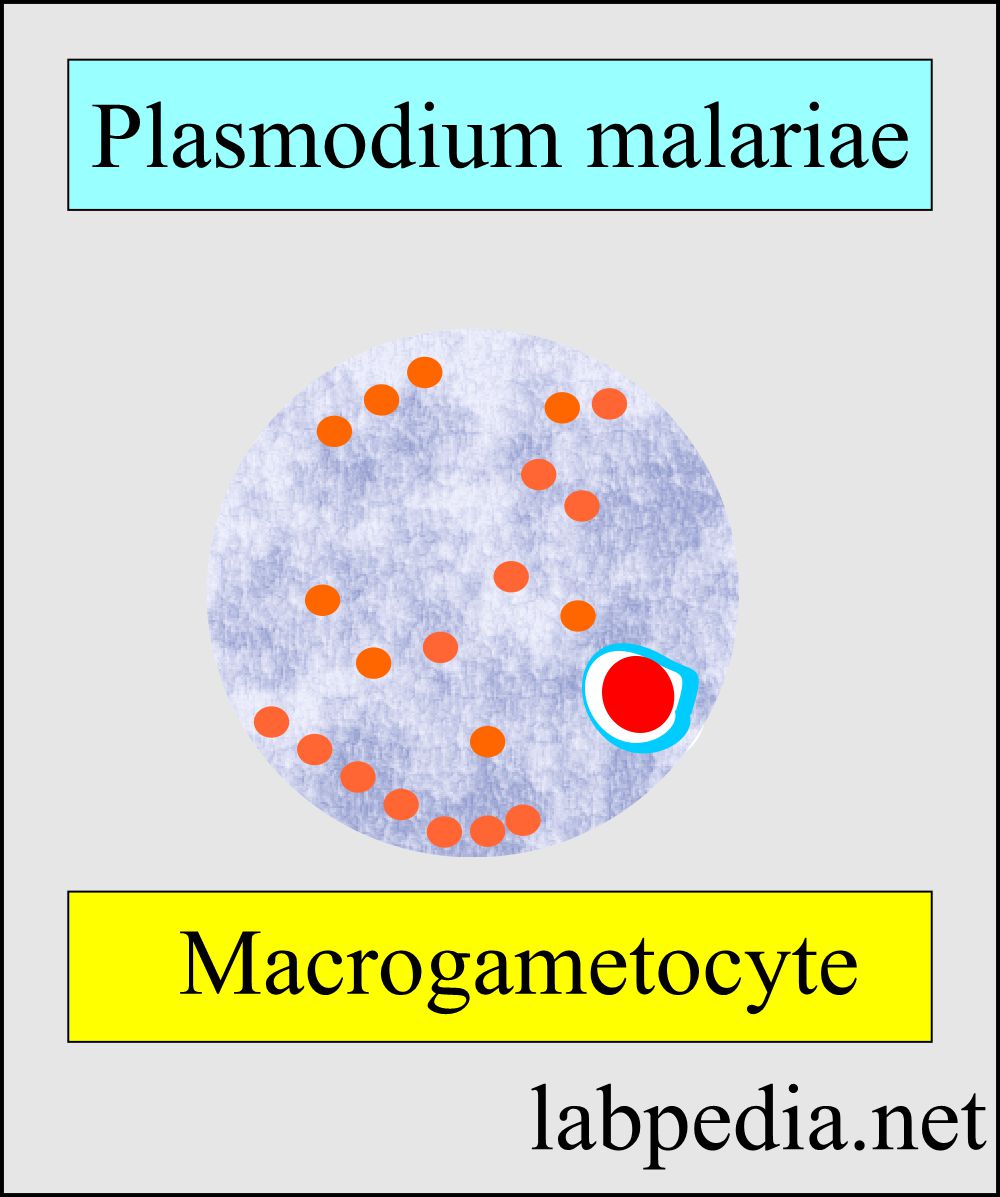
- Microgametes are similar to P. vivax except for one notable darker pigment, which is coarse.
- Macrogametocytes also have darker pigments and are more coarse.
- No Schuffner’s dots are seen.
Clinical presentations of Plasmodium Malariae
- There is an incubation period of 18 to 40 days.
- There is flue like symptoms.
- Cyclical paroxysms occur every 72 hours.
- There may be spontaneous recovery.
- No relapse is reported.
Diagnosis of Plasmodium Malariae
- History of the patient in suspected areas.
- Blood smear:
- Make a blood smear when the patient has a fever. Thin and Thick smears are made.
- The thick smear is more helpful in finding M.Parasites.
- The thin smear is good for identifying the type of malarial parasite.
- Collect blood 6 to 8 hourly till 48 hours to declare negative for malaria.
- Giemsa stain is the best choice.
- Serologic methods are based on immunochromatic techniques. Tests most often use a dipstick or cassette format and provide results in 2-15 minutes.
- Polymerase chain reaction (PCR): Parasite nucleic acids are detected using the PCR technique. This is more sensitive than smear microscopy. This is of limited value for diagnosing acutely ill patients because of the time needed for this procedure.
Mosquito control
- Try to eliminate breeding places:
- Fill the vacant land and pump out the water.
- Remove the junk and water-retaining debris.
- Destroy the larvae:
- Clean the drains.
- Try to remove algae from the ponds.
- Add larva-eating fish to the ponds.
- Use of the insecticide:
- The best example is DDT.
- Use of mosquito repellent:
- Pyrethroid repellent.
- N, N- diethyl meta tolbutamide.
- Use of mosquito nets.
- Use clothes to prevent mosquito bites.
- Train people for malaria prevalence.
- Train the people for the detection of malaria, treatment, and follow-up.
Treatment of plasmodium malariae
- Antimalarial drugs used are quinidine, chloroquine, primaquine, pyrimethamine, sulfadoxine, mefloquine, tetracyclines, and proguanil.
- Chloroquine is the drug of choice and is best for P. falciparum.
- This is effective for the erythrocytic stage and not for the liver stage.
- Must use primaquine to eradicate P. ovale and P. vivax.
- there are chloroquine resistant cases of P. falciparum.
- Amodiaquin, piperaquin and pyronaridine are close to chloroquin.
- In some areas, Amodiaquine is less toxic, cheap, and effective against chloroquine-resistant P. falciparum.
- Mefloquine is effective against choloquin resistant P. falciparum.
- Quinine and quinidine are still the first lines of therapy against P. falciparum.
- Primaquine is a synthetic drug and is the drug of choice for eradicating liver-stage from P. vivax and P. ovale.
- Antibiotics and Inhibitors of folate synthesis are slow-acting antimalarial drugs.
- Halofantrine and Lumefantrine are related to quinine and effective against the erythrocytic stage.
- Malaria drug-resistant strains are emerging.
Questions and answers:
Question 1: How many days are needed for the exoerythrocytic cycle?
Question 2: How many merozoites are seen in the schizonts of plasmodium malariae?