Malarial Parasite: – Part 1 – Malarial parasite, Plasmodium Life Cycle and Diagnosis
Malarial parasite
Sample for Malarial parasite
- Malarial parasites (MP) may be diagnosed with a fever from a patient’s blood smear.
- The best time to make a smear is during shivering.
- Make thick and thin blood smears.
- Serum needed for a Serological method and for PCR.
Indication for Malarial parasite
- The diagnosis of the malarial parasite.
Parasitology of Malarial parasite
- This word malaria is the Italian word that means mala; aria means bad air.
- The plasmodium grows in the swamp-bred mosquito.
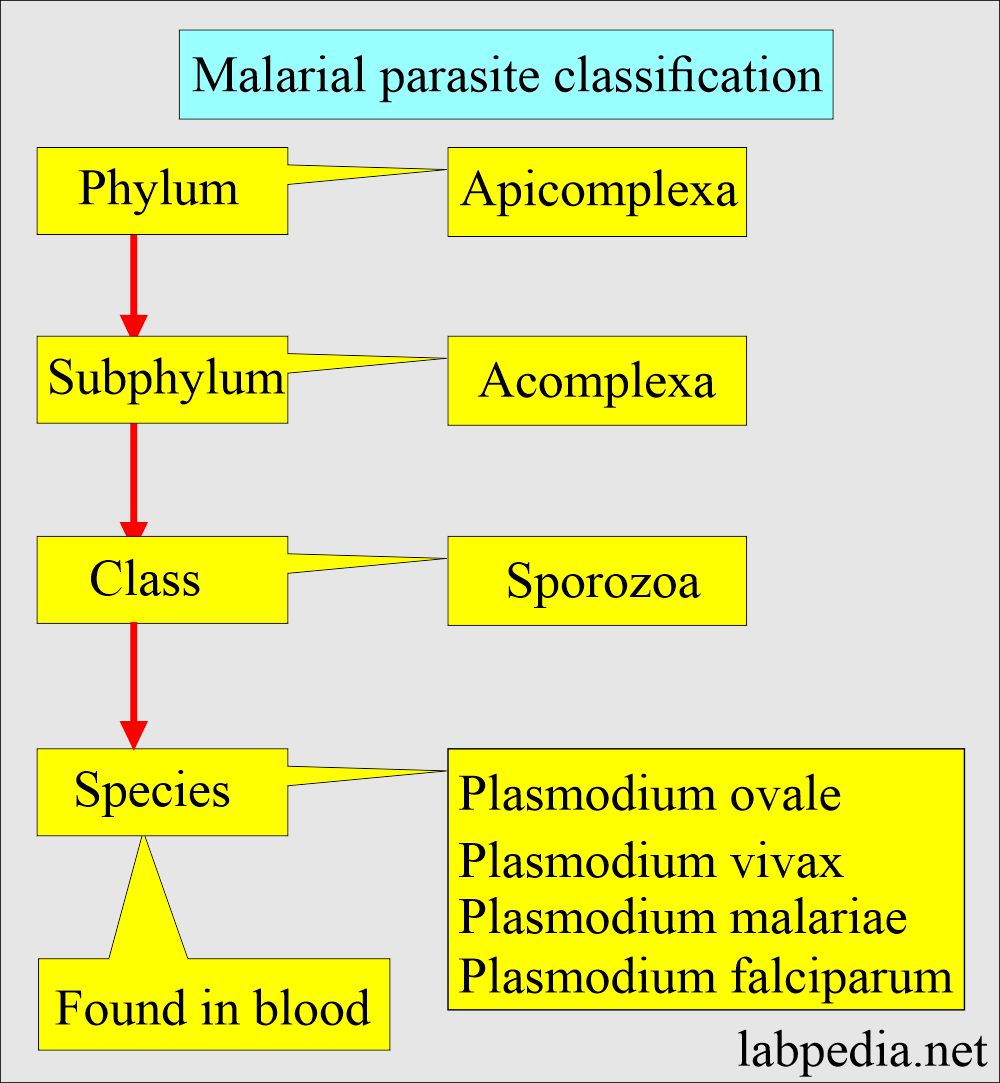
- Malaria is caused by protozoan parasites called Plasmodia and belonging to the Plasmodiidae family.
- Types of malaria parasites are :
- P. falciparum.
- P. vivax.
- P. ovale.
- P. malariae.
- A fifth one, P. knowlesi.
Vector of malarial parasite:
- All the Plasmodium species causing malaria in humans are transmitted by mosquito species of the genus Anopheles.
Spread of malarial parasite:
- Sporozoites from the saliva of a biting female mosquito are transmitted to either the blood or the lymphatic system of the recipient.
- Malaria spreads through:
- Mosquito bite.
- Transfusion malaria from the contaminated transfused blood.
- By sharing contaminated needles and syringes, mostly the drug abusers.
- Congenital malaria is rare.
Plasmodium’s different shapes:
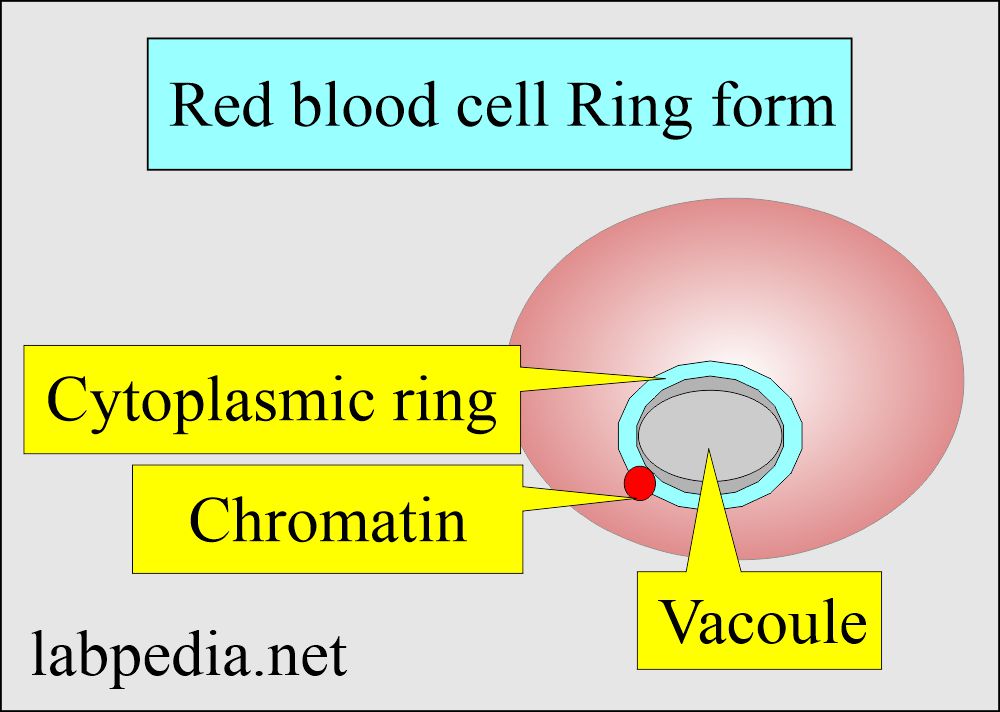
Ring form:
- It is an early trophozoite.
- This is a ring-like malarial parasite following the invasion of RBCs.
- Giemsa stain shows it as a blue stain cytoplasmic circle connected to a red chromatin dot.
- The space inside the ring is known as the vacuole.
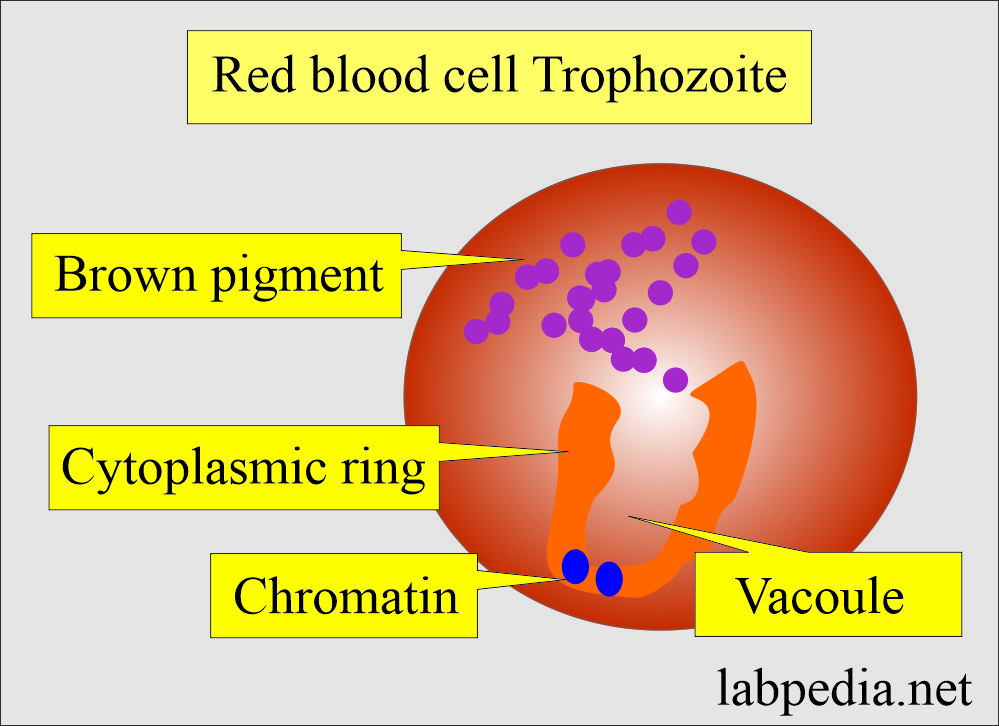
Trophozoites:
- The shape varies according to the type of malarial parasite.
- There are a cytoplasmic circle and a chromatin dot.
- More space is taken by the developing trophozoites.
- Pigments are brown in color.
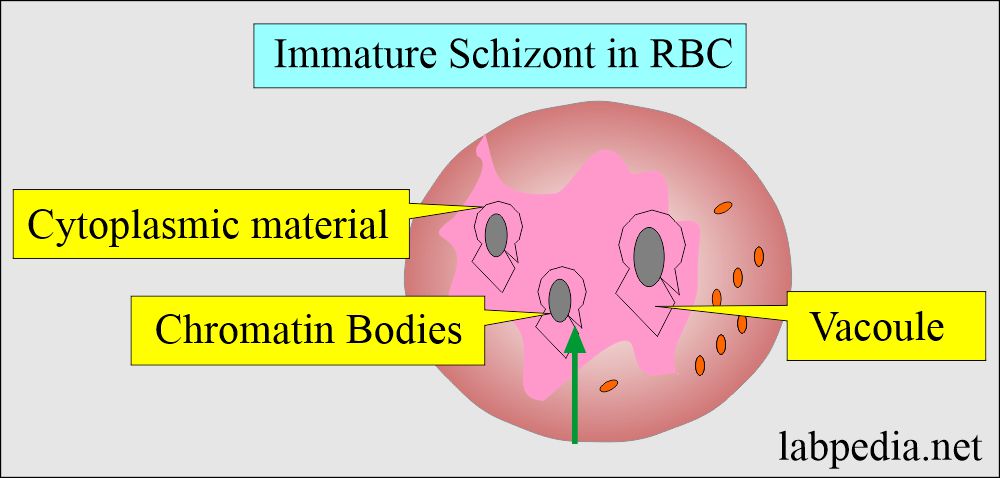
Immature schizonts:
- There is active chromatin replication.
- Visible cytoplasmic material surrounds the growing chromatin.
- Pigments are often brown.
- It occupies more space in the RBC.
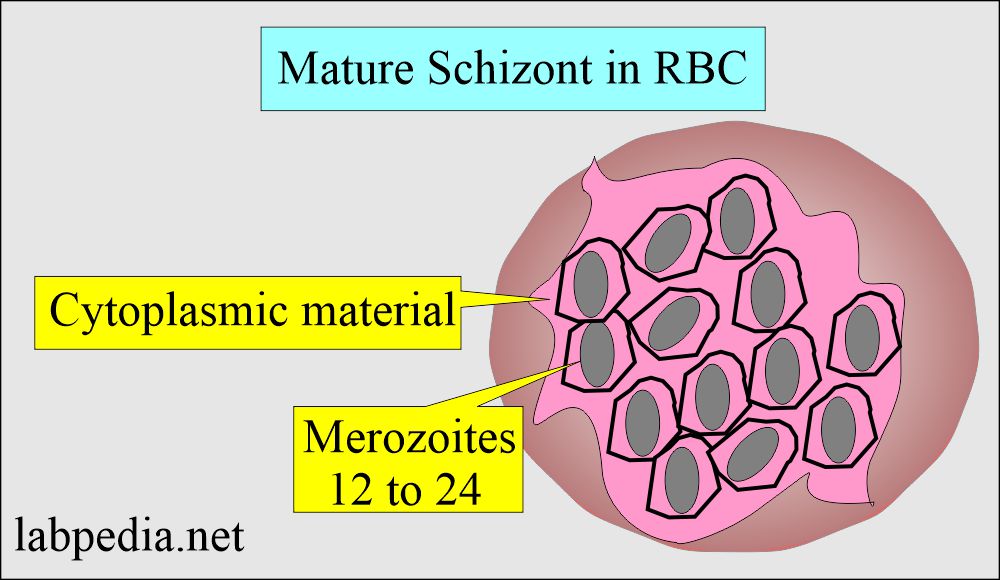
Mature Schizonts:
- These are characterized by the presence of merozoites.
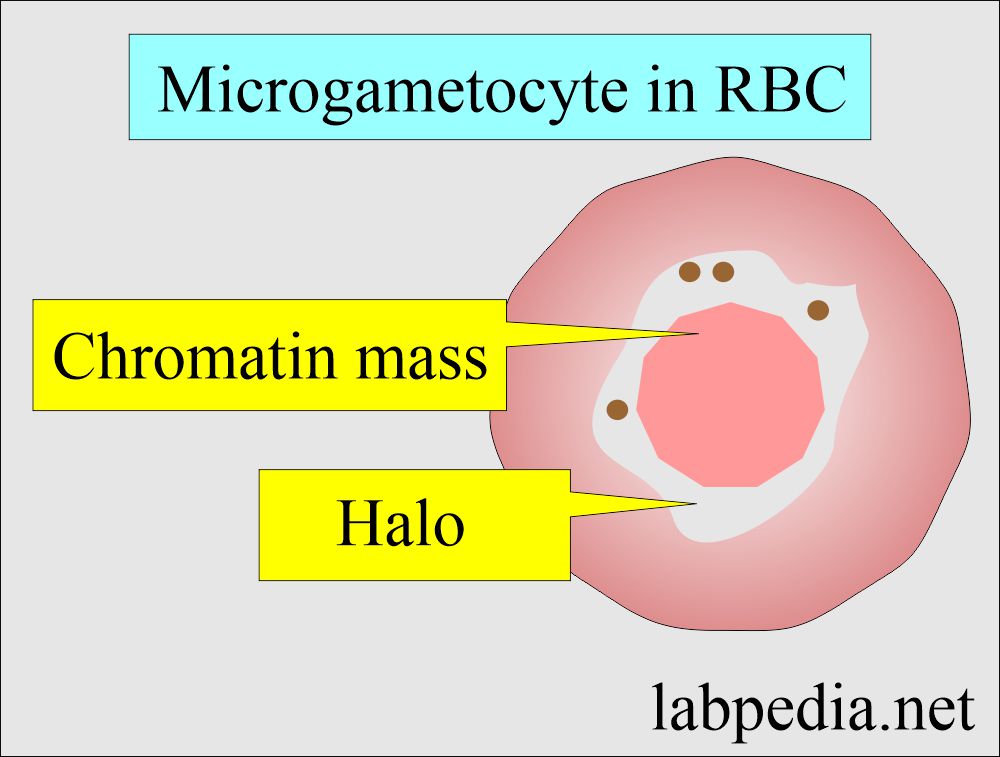
Microgametocytes:
- Plasmodium falciparum is crescent-shaped; in others is typically round in shape.
- There is a large diffuse chromatin mass that stains pink to purple.
- Chromatin mass is surrounded by a colorless pale halo.
- Pigments are usually visible.
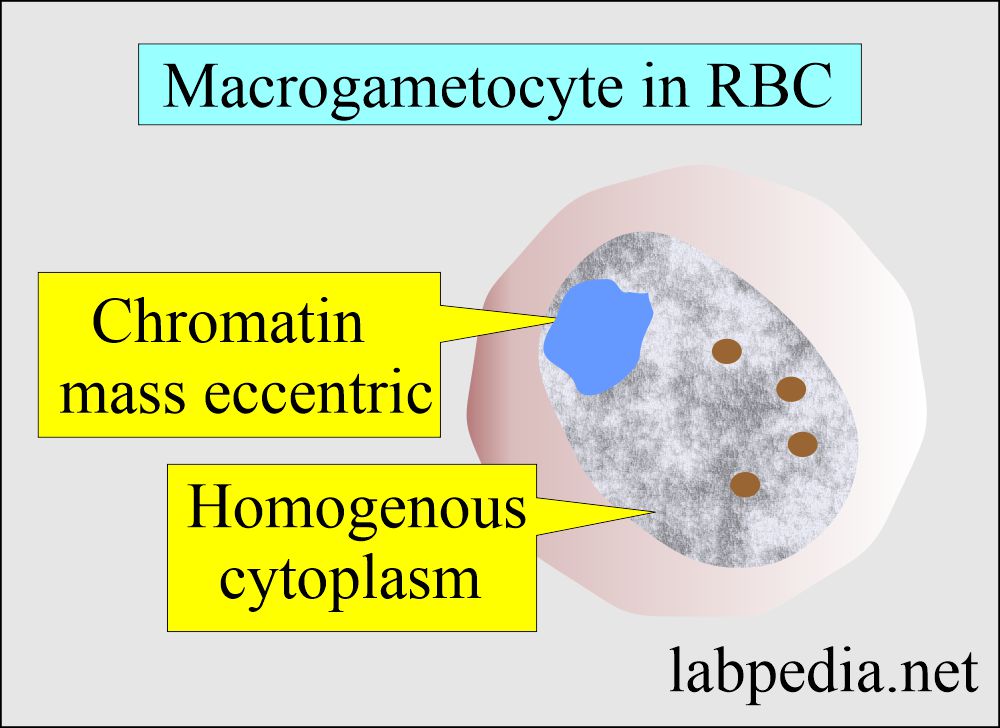
Macrogametes:
- These are round to oval in shape, with the exception of P. falciparum, which is crescent in shape.
- Chromatin is surrounded partially or completely by the cytoplasm.
- Pigments are also present.
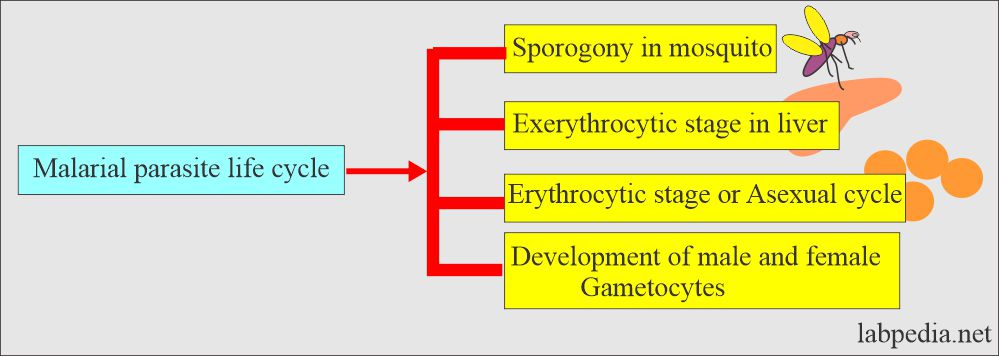
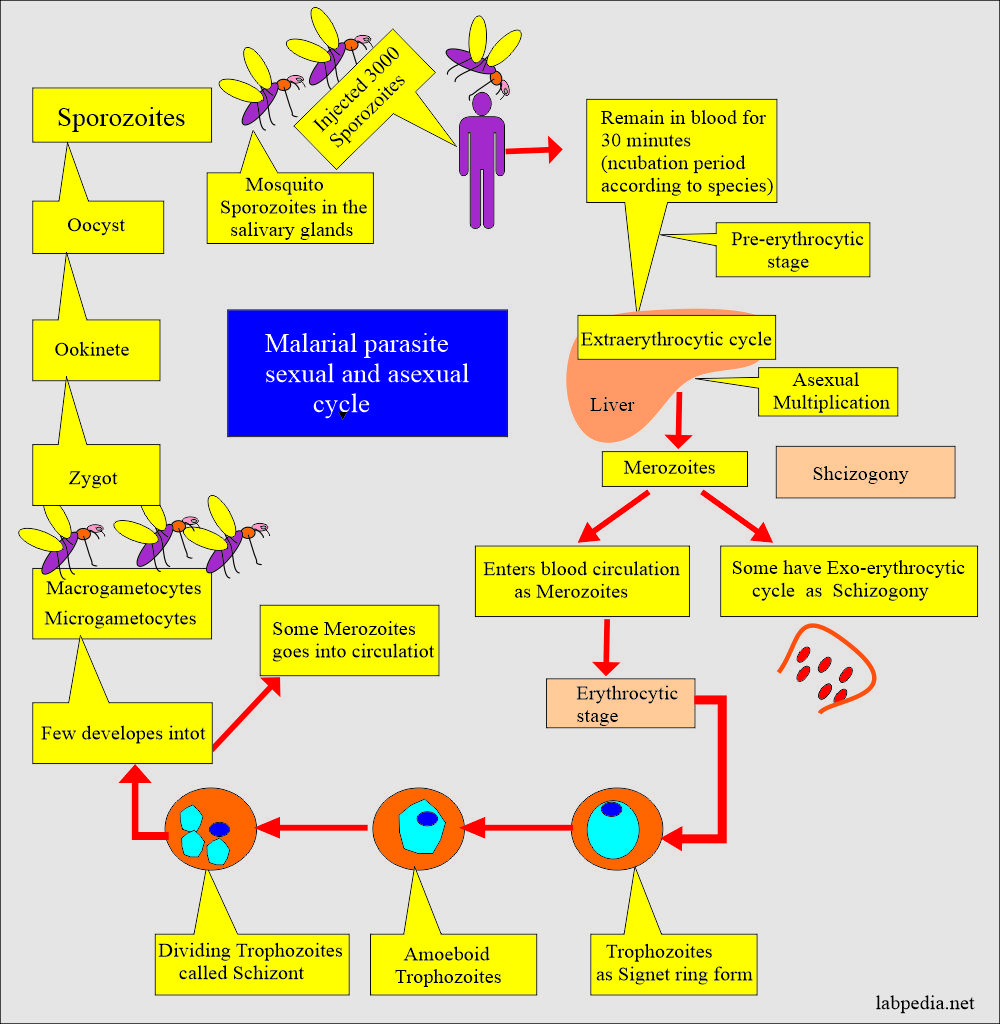
Lifecycle of malarial parasite:
Asexual cycle:
- The majority of sporozoites migrate to the liver and invade hepatocytes.
- Initially, elongated sporozoite has transformed into a rounded form.
- This rounded form then matures within the hepatocyte to a schizont containing many merozoites.
- This cycle takes 5 to 16 days.
- Merozoites leave the liver and enter the blood; this is an asexual cycle.
The sexual cycle:
- It starts when the mosquito sucks the blood from the patients.
- Micro and macrogametocytes in the stomach of a mosquito combine and form a zygote.
- This forms oocyst and sporozoites.
- Sporozoites are injected into humans containing merozoites.
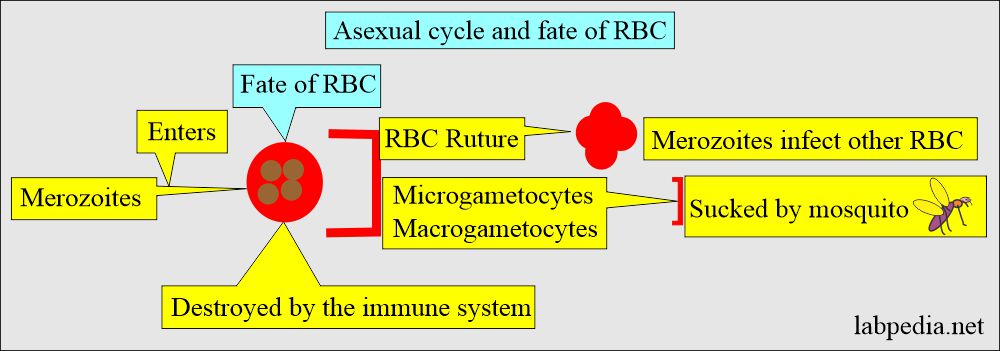
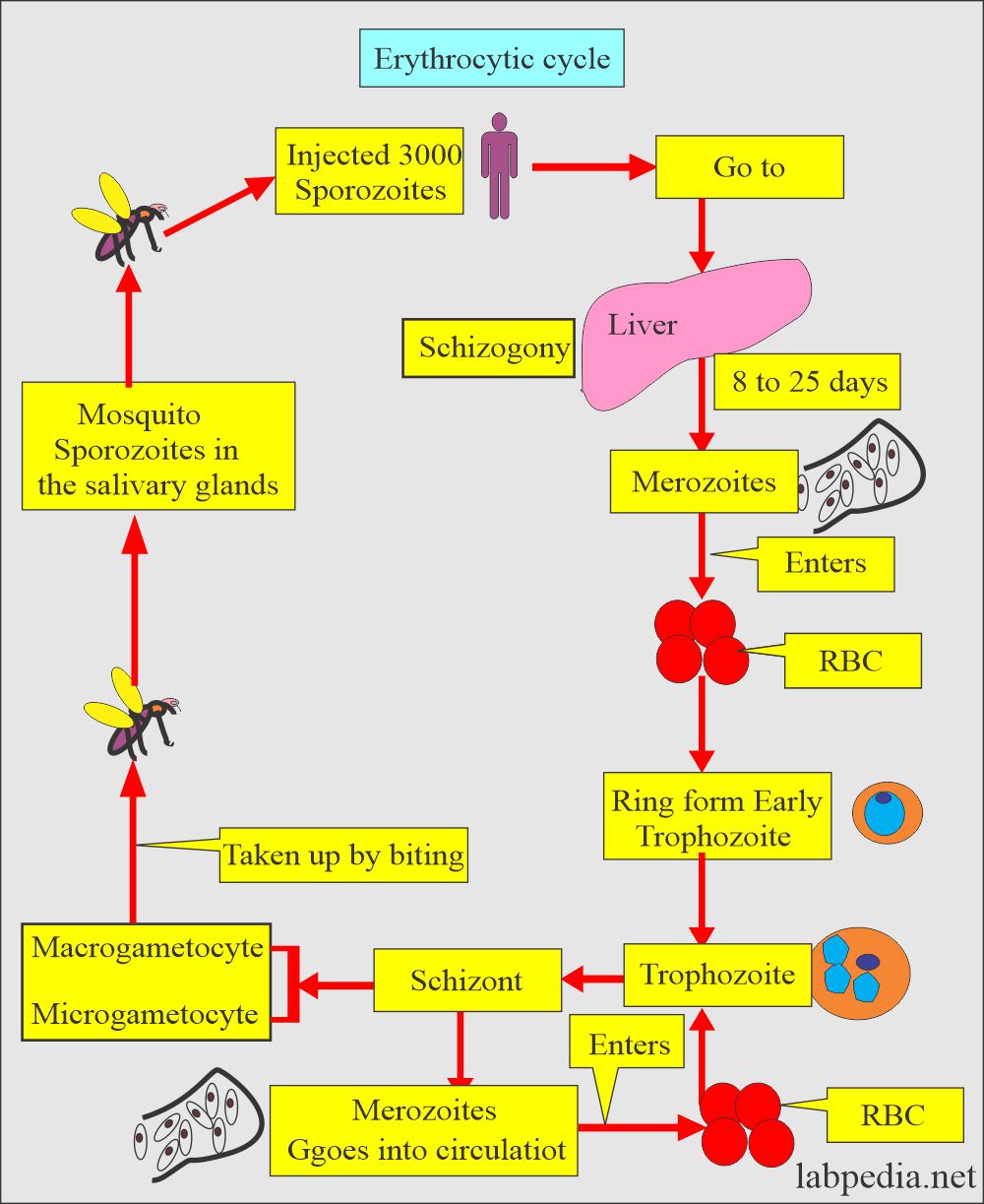
RBCs cycle (Erythrocytic cycle) Asexual cycle:
- Now Merozoites enter the RBCs and start the Asexual cycle.
- Produce more merozoites. This cycle repeats for 1 to 3 days.
- This multiplication can result in thousands of parasite-infected cells in the host bloodstream.
- The patient may develop signs and symptoms of illness and complications of malaria.
- The complication of the malaria parasite, if not treated then it may last for months.
- Some of the merozoites transform into a sexual form called male and female gametocytes.
- These gametocytes circulate in the blood and are taken up by the biting mosquito.
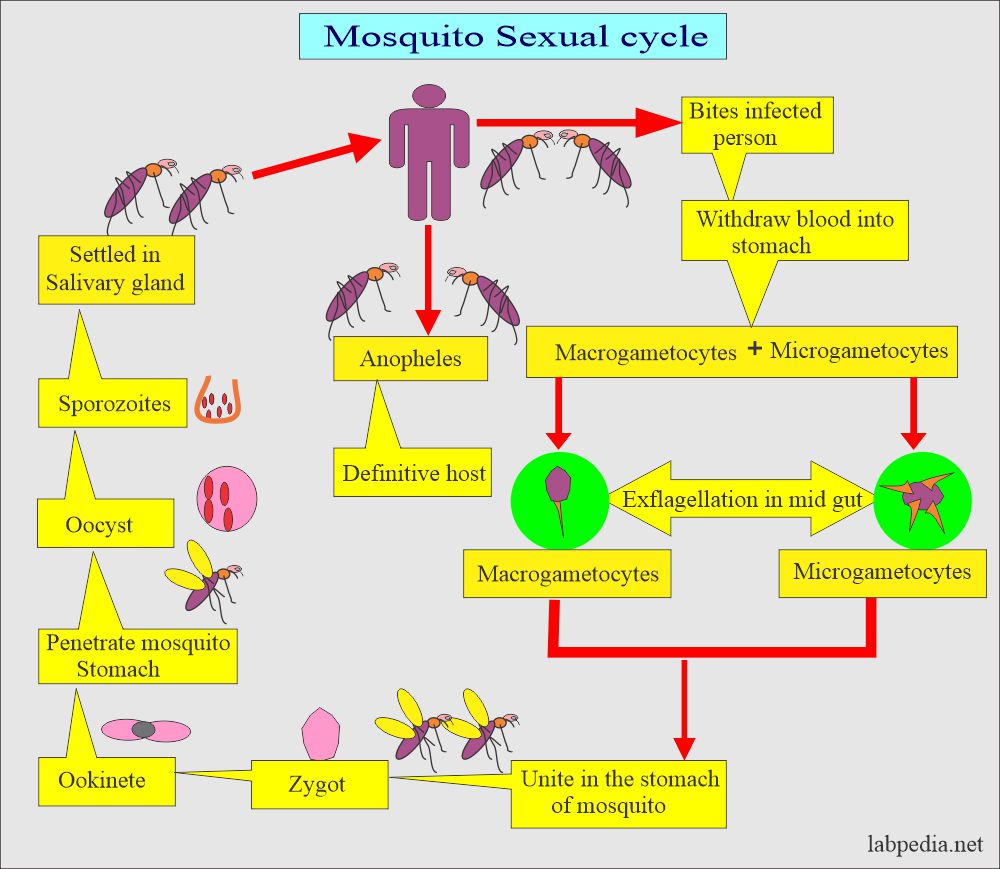
The life cycle in the mosquito (Sexual cycle):
- When the mosquito bites the infected humans, it sucks the blood, and these gametocytes go along the blood.
- In mosquito RBCs, burst and gametocytes are released. These will get into more mature forms of Gametes.
- Male and female gametes fuse to form diploid zygotes.
- Zygotes develop into actively moving ookinetes that burrow into the mosquito midgut wall and form oocysts.
- Growth and division of each oocyst produce thousands of active haploid forms called sporozoites.
- After 8-15 days, the oocyst bursts, releasing sporozoites into the body cavity of the mosquito, from which they travel to and invade the mosquito’s salivary glands.
- Mosquito is ready to infect humans.
Clinical presentation of malaria parasite:
- The Typical patient is initially asymptomatic following the mosquito bite.
- Once the erythrocytic phase starts, many RBCs rupture, releasing merozoites and toxic material.
- This is the time when patients get their first attack of malaria as:
- First, chills for 10 to 15 minutes and then fever for 2 to 6 hours or more.
- When the fever settles to normal, then the patient gets profuse sweating.
- This cycle may vary with the type of malaria.
- This is the time when patients get their first attack of malaria as:
- The patient may have a headache, lethargy, anorexia, nausea, and vomiting.
- There may be diarrhea.
- There is anemia.
- There may be involvement of the central nervous system.
- Kidney involvement may lead to nephrotic syndrome.
Complications of Malarial parasite:
- The patient may have :
- Cerebral malaria.
- Anemia.
- Organ failure.
- Some patients may have respiratory difficulties.
- Rarely there may be low blood sugar levels.
Diagnosis of malarial parasite:
- History of the patient in suspected areas.
- Blood shows thrombocytopenia, and relative monocytosis is a common pattern.
- There is leucopenia.
- Bone marrow shows erythroid hyperplasia.
- Blood smear:
- Make a blood smear when the patient has a fever. Thin and Thick smears are made.
- The thick smear is more helpful in finding M.Parasites.
- A thick smear is sensitive to 2 parasites/1,000,000 uninfected RBCs.
- The thin smear is good for identifying the type of malarial parasite.
- Collect blood 6 to 8 hours weekly for 72 hours to declare negative for malaria.
- Giemsa stain is the best choice.
- Serologic methods are based on immunochromatic techniques. Tests most often use a dipstick or cassette format and provide results in 2-15 minutes.
- Polymerase chain reaction (PCR): Parasite nucleic acids are detected using the PCR technique. This is more sensitive than smear microscopy. This is of limited value for diagnosing acutely ill patients because of the time needed for this procedure.
- Flow cytometry to find infected RBCs.
- In the late stages, may see agranulocytosis and purpura may occur late.
Mosquito control of malarial parasite:
- Try to eliminate breeding places:
- Fill the vacant land and pump out the water.
- Remove the junk and water-retaining debris.
- Destroy the larvae:
- Clean the drains.
- Try to remove algae from the ponds.
- Add larva-eating fish to the ponds.
- Use of the insecticide:
- The best example is DDT.
- Use of mosquito repellent:
- Pyrethroid repellent.
- N, N- diethyl meta tolbutamide.
- Use of mosquito nets.
- Use of clothes to prevent mosquito bites.
- Train people for malaria prevalence.
- Train the people for the detection of malaria, treatment, and follow-up.
Prevention of malarial parasite:
- No vaccine is available.
- Give prophylactic anti-malarial drugs.
- Use a mosquito net.
- Use mosquito repellant.
Treatment of malarial parasite infestation:
- Antimalarial drugs are quinidine, chloroquine, primaquine, pyrimethamine, sulfadoxine, mefloquine, tetracyclines, and proguanil.
- Chloroquine is the drug of choice and is best for P. falciparum.
- This is effective for the erythrocytic stage and not for the liver stage.
- Must use primaquine to eradicate P. ovale and P. vivax.
- there are chloroquine resistant cases of P. falciparum.
- Amodiaquin, piperaquin and pyronaridine are close to chloroquin.
- Amodiaquine is less toxic, cheap, and effective against chloroquine-resistant P. falciparum in some areas.
- Mefloquine is effective against choloquin resistant P. falciparum.
- Quinine and quinidine are still the first lines of therapy against P. falciparum.
- Primaquine is a synthetic drug and is the drug of choice for eradicating liver-stage from P. vivax and P. ovale.
- Antibiotics and Inhibitors of folate synthesis are slow-acting antimalarial drugs.
- Halofantrine and Lumefantrine are related to quinine and effective against the erythrocytic stage.
- Malaria drug-resistant strains are emerging.
Characteristic features of various forms of the Malarial parasite
| Malaria type | Stages | Infected RBC size | Trophozoite | Scuffer stippling | GAMETOCYTES | Pigments (hematin) | Schizont nuclei |
| P. vivax | All | enlarged | small and may become amoeboid | present | rounded | light brown | 12 to 24 |
| P. Ovale | All | enlarged | small, with large chromatin | present | rounded | dark brown | 6 to 12 |
| P. malariae | All | normal | small with dense cytoplasm, rarely band form | absent | rounded | dark brown | 6 to 12 |
| P. falciparum | ring form | normal | smallest, sometimes multiple, often double chromatins | absent | banana-shaped | black | rarely |
Typical features of Malarial parasite
| Clinical parameters | P. falciparum | P. vivax | P. ovale | P. malariae |
| Incubation period | 8 to 11 days | 7 to 10 days | 7 to 10 days | 18 to 40 days |
| Fever pattern | Continuous, quotidian, or remittent | Irregular or quotidian | Irregular or quotidian | usually regular after 72 hours. |
| Prodromal symptoms | Influenza-like | Influenza-like | Influenza-like | Influenza-like |
| The periodicity of symptoms | 36 to 48 hours | 44 to 48 hours | 48 to 50 hours | 72 hours |
| The severity of the initial attack | Severe 16 to 36 hours | moderate to severe, 10 hours | mild for 10 hours | moderate to severe 11 hours |
| Duration without treatment | 2 to 3 weeks | 3 to 8 + weeks | 2 to 3 weeks | 3 to 24 weeks |
| CNS involvement | very severe ++++ | ± | ± | ± |
| Anemia | very severe ++++ | ++ | + | ++ |
| Kidney involvement | + | ± | – | +++ |
| Red blood cell | normal size | larger than normal, Schuffner’s dots are seen | larger than normal, schuffner’s dots are often seen | about normal or slightly smaller |
| Early trophozoite | about 1/5 diameter of RBC, chromatin is a small dot | about 1/3 diameter of RBC with heavy chromatin dots | Like vivax and malariae | single, heavy chromatin dot |
| Trophozoite mature | usually not seen in peripheral blood | as a large mass of chromatin, fine brown pigments | Chromatin is elongated and less definite. | |
| Schizont | 8 to 24 or more merozoites | 12 to 24 merozoites | 4 to 16 but more common 8 merozoites | 6 to 12 but usually 8 or 10 merozoites |
| Macrogametocyte |
size like microgametocyte. Chromatin more compact |
The cytoplasm stains dark blue, and chromatin is more compact. | Abundant pigments and coarser, dark brown granules | |
| Microgametocyte | Crescent-shaped, chromatin is diffuse, pink, cytoplasm pale blue | Round or oval, almost fill the RBC, chromatin is diffuse in large masses, pink, no vacuoles | Like vivax but smaller | like vivax but smaller and pigments more prominent |
| Stages development in the mosquito | 10 to 12 days at 27 °C | 10 days at 25 °C to 30 °C | 14 days at 27 °C | 25 to 28 days at 24 °C |
Questions and answers:
Question 1: Which malarial have banana shape gametocyte?
Question 2: Is there a vaccination for malaria?