Chapter 19: Autoimmune Diseases:- Sjogren’s Syndrome (SS)
SJOGREN’S SYNDROME (SS)
Definition: – This is a chronic inflammatory condition of unknown etiology, mainly affecting lacrimal and salivary glands, characterized by:-
- Dry eyes – Keratoconjunctivitis sicca.
- Dry mouth – Xerostomia.
- Involvement of other excretory glands.
Types:- Sjogren’s Syndrome (SS) is of two types.
- Primary SS – When disease occurs alone.
- Secondary SS – When it is associated with rheumatoid arthritis, SLE, and less frequently with systemic sclerosis.
Age: It involves middle-aged females 40 to 60 years of age. 90% of patients are women with a mean age of 50 years.
Sex: It is more common in females with a male: female ratio of 1:9.
Major Immunologic Features
- There is an infiltrate of lymphocytes and plasma cells in the involved tissue.
- There is an increased level of Immunoglobulin (hypergammaglobulinemia) and also the presence of RF and ANA.
- Presence of autoantibody against salivary duct cell antigen.
Etiology and Pathogenesis
- Etiological factors considered are:
- Infection.
- Genetic factors.
- Abnormalities in the immune regulations.
- HLA-association:- There is a strong association between HLA-B8 and HLA-DR3.
- The damage to tissue is not clear whether due to T-L or B-L.
- There may be functional defects in:
- B-L.
- T-L.
- Macrophagic cells.
- The activation of the above cells may start because of:
- Genetic defect.
- Viruses-like EBV.
- Deranged immune regulatory system.
- The inflammatory cells are mainly T-L and-B-lymphocytes, with the predominance of CD4+ There may be few CD8+ cells. All these express markers of activation and these Th-2 cells may stimulate B-L.
- There is clear evidence for the overactivity of B-lymphocytes, but it is not known that it is due to B or T lymphocytes.
- There is the presence of other autoantibodies in SS:
- 70% shows RF.
- 50-80% shows ANA.
- 25% LE cell Positive.
- SS-A (anti- Ro) against the extractable nuclear antigen.
- SS-B (anti-La) against the extractable nuclear antigen.
All these autoantibodies may be due to activation of-B-L because there is also hypergammaglobulinemia.
Signs & Symptoms
- There is blurred vision, burning, and itching of the eyes.
- There is difficulty in swallowing due to thick secretions (Xerostomia).
- Recurrent salivary glands pain and swelling.
- Oral mucosa may show atrophy.
- There is dysphagia and atrophic gastritis can also be seen.
- There is an enlargement of the parotid gland in 50% of the cases.
- 25% show extraglandular involvement like kidney, lung, CNS, and muscles.
- Sometimes they have fatigue, low-grade fever, arthralgias, and myalgias.
- There are hoarseness and chronic cough.
- There is an increased incidence of infection.
- The dryness of the vagina leads to pareunia and itching.
- Extraglandular involvement leads to interstitial pneumonitis and fibrosis.
- CNS and peripheral nerves may also be involved and show vasculitis.
- Kidneys may show renal tubular acidosis.
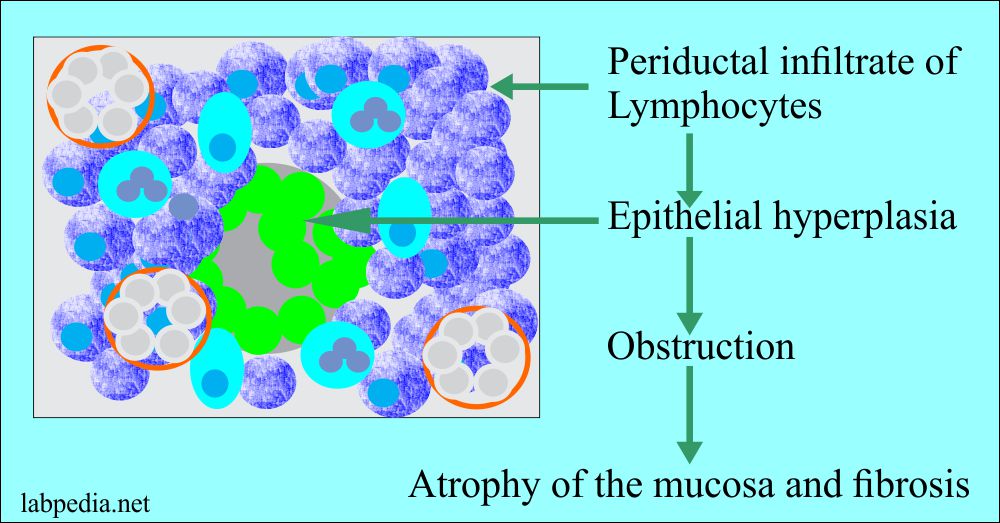
Microscopic examination:
It shows periductal and perivascular lymphocytic infiltrate in the early stages.
Then there is epithelial hyperplasia which leads to obstruction. Lymphocytic infiltrate increases with the appearance of fibrosis. There is atrophy of mucosa. The lymphocytic infiltrate sometimes gives a picture of Pseudolymphoma.
Diagnosis
- There is mild anemia and raised ESR.
- ANA is positive in ≥70% of the patients.
- SS-A (anti-Ro) and SS-B (anti-La) are considered serological markers. These are positive around 80% to 90% of the cases.
- Rheumatoid factor (RF) is frequently positive in around 90% of the cases.
- Serum gamma globulins are raised in 50% of the cases.
- Schirmer’s test demonstrates a decrease in tear flow.
- Eye-Slit lamp examination of the eye with Bengal staining shows typical punctate corneal ulcers and these are highly diagnostic.
- Lip biopsy shows lymphocytic infiltration of the salivary glands.
Complication
- Sjogren’s syndrome gives 40 fold increased risk for lymphomas and mostly these are B-cell lymphoma.