Diabetes Mellitus:- Part 7 – Diabetic Ketoacidosis and Ketone Bodies
Diabetic Ketoacidosis
What sample for Diabetic Ketoacidosis is needed?
- The ketones can be detected in blood and urine.
What are the precautions for Diabetic Ketoacidosis?
- The false-positive test may be seen in some medications.
- Prolonged exposure of the strips to air gives a false-negative result.
How will you Define diabetic ketoacidosis?
- This is an acute life-threatening metabolic acidosis due to uncontrolled diabetes mellitus.
- It is mostly due to type 1 and less frequently by type 2.
- It is a decompensated stage of intercurrent illness and severe insulin deficiency.
- There is excess hormone-producing glucose.
- Normally, no ketones are present in the urine.
- Diabetic ketoacidosis is due to Ketone bodies in the blood and the urine.
- There is a presence of ketones in the blood, which are toxic acids.
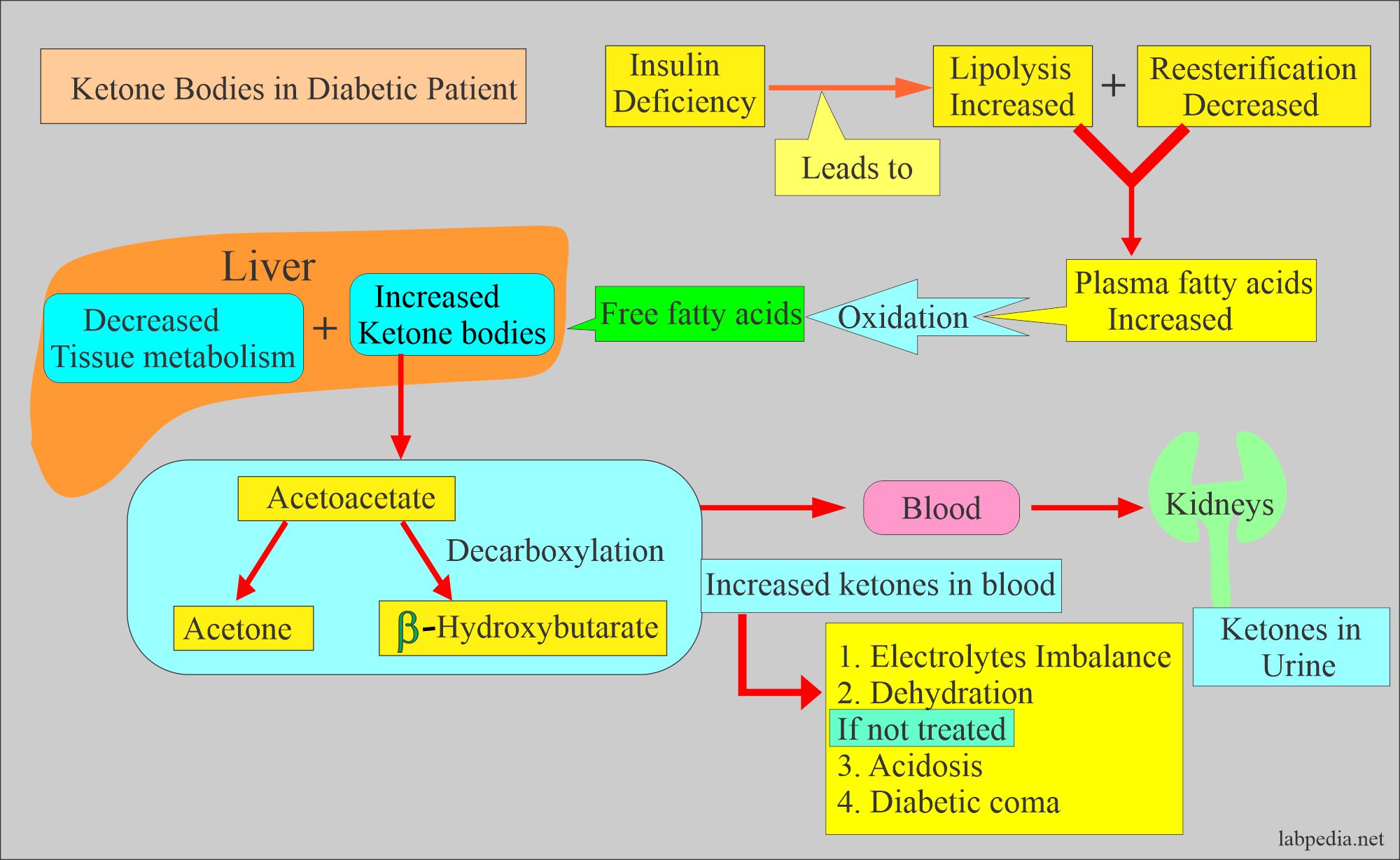
Pathophysiology of Diabetic Ketoacidosis
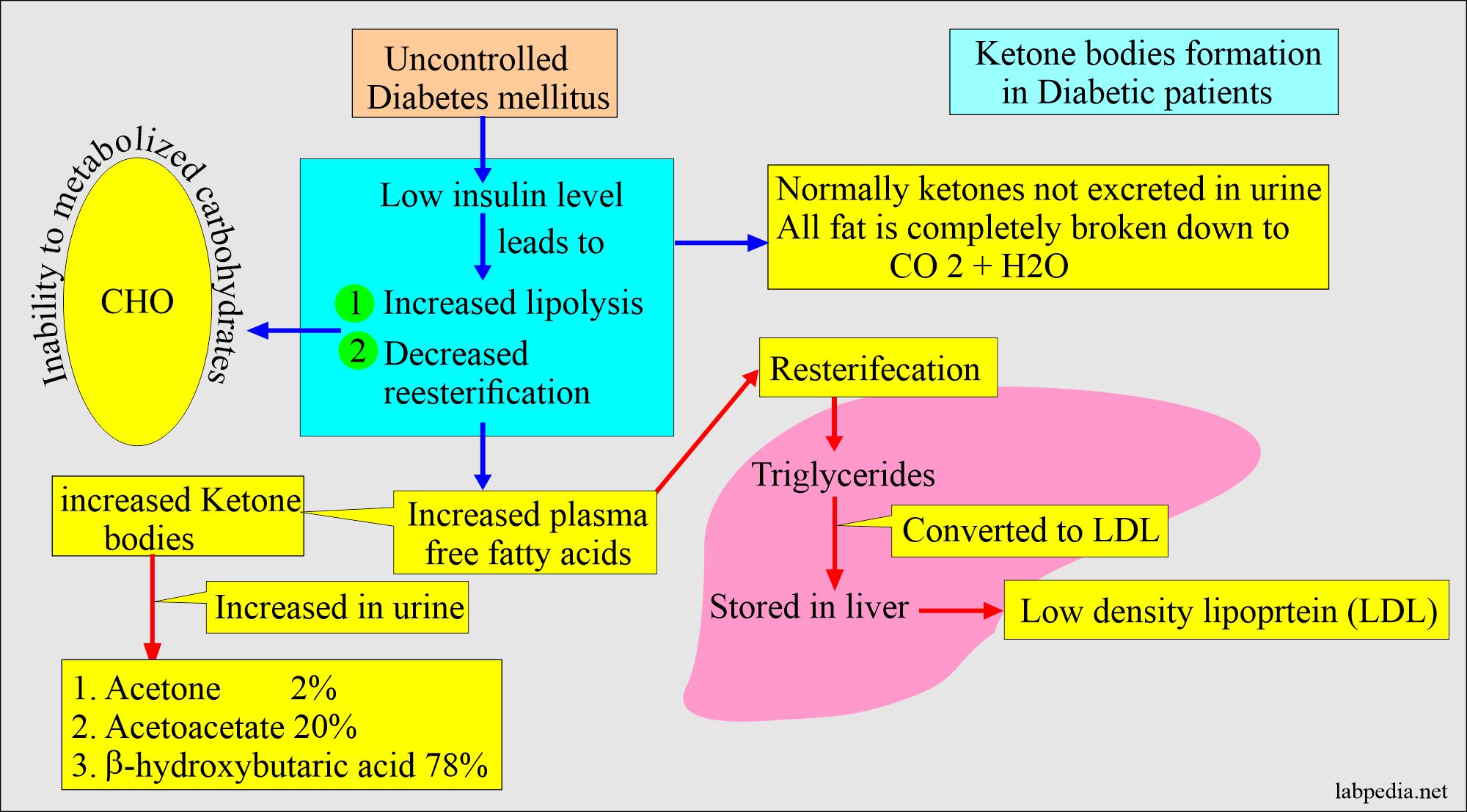
- This is a complication in diabetic patients with hyperglycemia and massive fatty catabolism.
- The primary substrate for ketone body formation is free fatty acids from adipose tissue.
- This is due to the lack of insulin in uncontrolled diabetes mellitus.
- These free fatty acids are substrates for the formation of ketone bodies.
- When reesterified in the liver, these free fatty acids give rise to triglycerides and low-density lipoproteins.
- When the body can not utilize carbohydrates or glucose, it can not enter the cells.
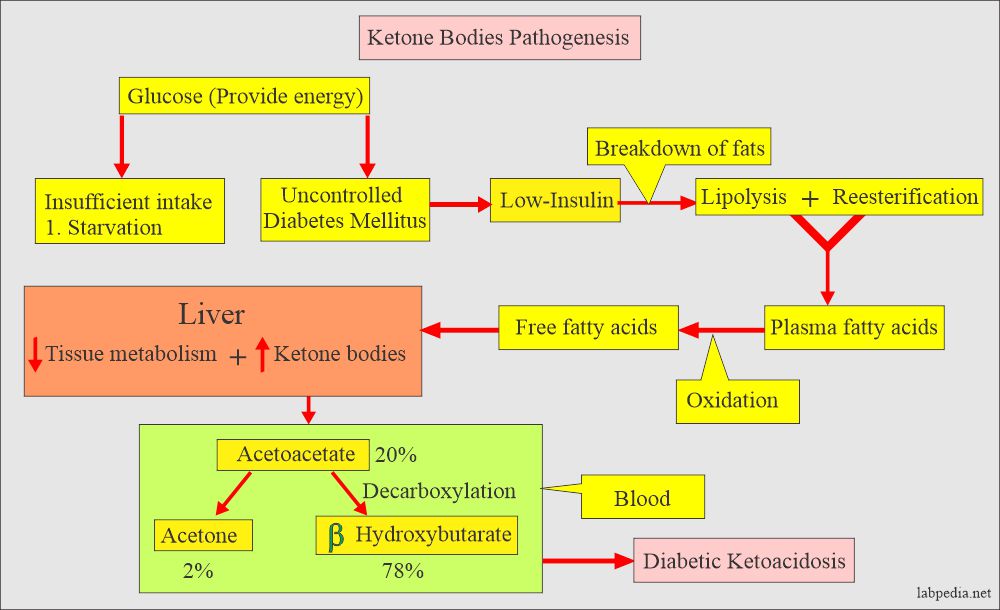
What is the mechanism of ketone body production?
- Glucose provides energy to the body. During starvation or uncontrolled diabetes mellitus, the energy is supplied by the breakdown of fats.
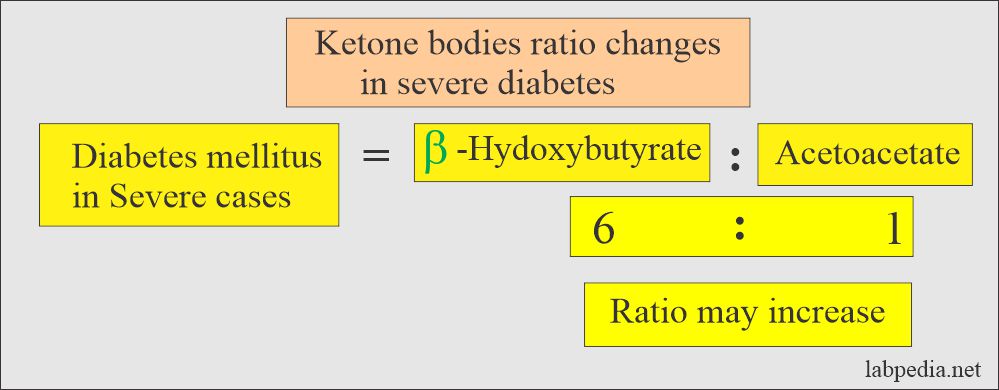
- In the blood samples, mainly 78% is beta-hydroxybutyric acid, and acetone is hardly 2%.
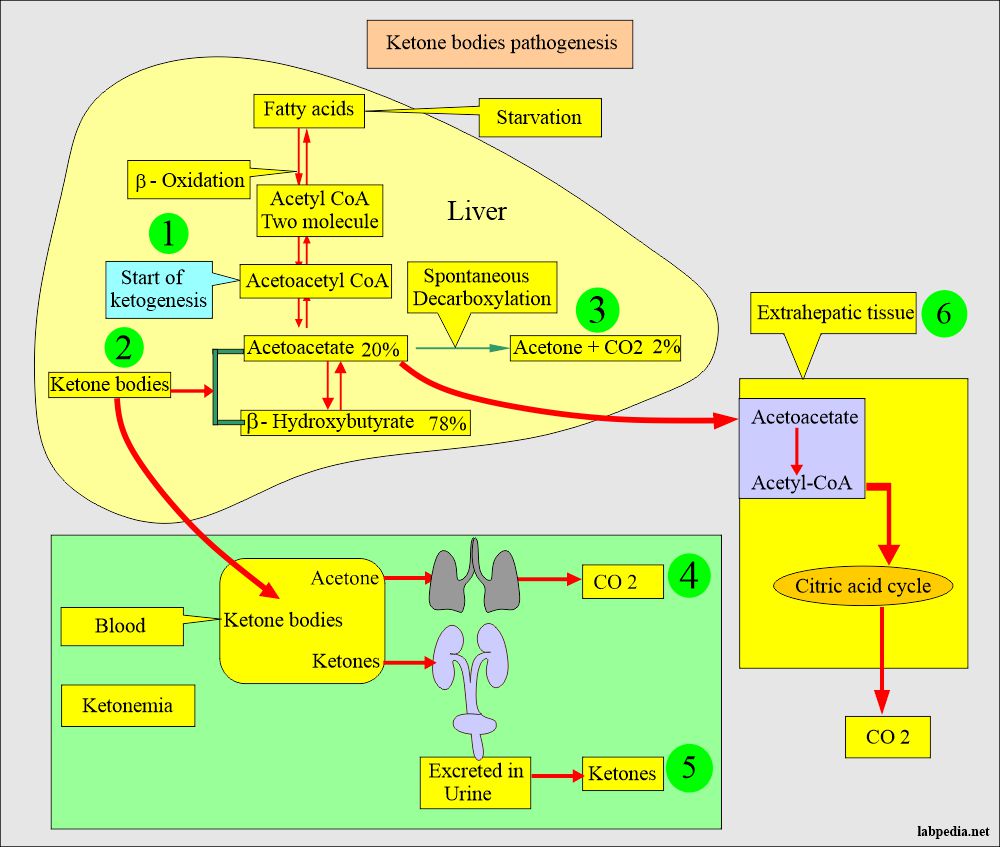
- Ketones are formed when fats provide energy to the body. The enzymes responsible for forming ketone bodies are present in the mitochondria.
- Acetyl-CoA from acetoacetyl-CoA by the β-oxidation.
- Acetoacetyl-CoA- CoA is the starting point of ketogenesis.
- Acetoacetate is formed from the acetoacetyl-CoA in the liver.
- In the extrahepatic tissue, acetoacetate is activated by acetoacetyl-CoA.
- Now acetoacetyl-CoA- CoA is split into acetyl-CoA by thiolase, is oxidized in the citric acid cycle, and produces CO2.
- In most cases of ketonemia, increased ketone bodies are formed in the liver and are not dependent upon the utilization of ketone bodies in the extrahepatic tissue.
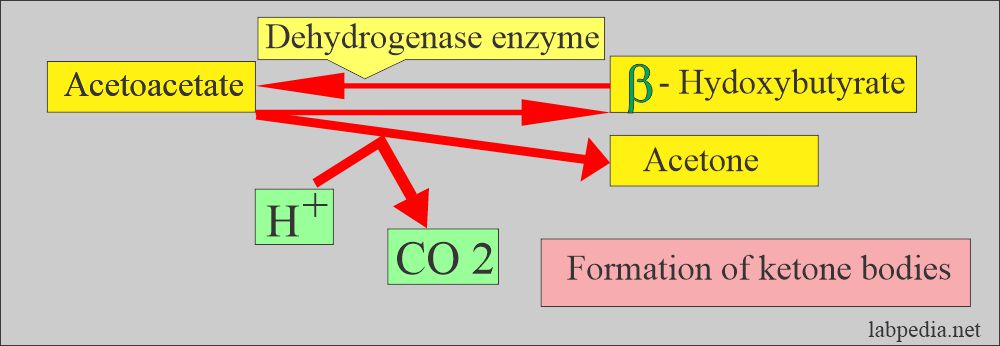
- Ketone bodies are:
- Acetoacetate.
- β-hydroxybutyrate.
- Acetones.
- ketone bodies are the end product of fatty acid breakdown.
- The presence of ketone bodies in the urine indicates poorly controlled diabetes mellitus.
How will you define Ketonemia and ketonuria?
- It is called ketosis when the body can not utilize the ketone bodies produced in excess.
- These are excreted in the urine and are called ketonuria. There is the excretion of ketones more than traces.
- The elevated level of ketones in the blood is called ketonemia.
- This overproduction of keto acids leads to acidosis or lowers blood pH.
- Ketone bodies are toxic to the brain; if present in abundance in the blood, these will lead to coma.
- Diabetic ketoacidosis is life-threatening metabolic acidosis due to uncontrolled diabetes mellitus, usually seen in type 1 and less common in type 2.
What are the Signs and Symptoms of diabetic ketoacidosis?
- This condition is seen in carbohydrate deficiency, starvation, or frequent vomiting.
- The patient will have a thirst and a dry mouth.
- Increased frequency of urine.
- There is easy fatigue.
- There may be nausea, vomiting, and abdominal pain.
- There is a fruity odor breathe.
- Difficulty in concentration and confusion.
- This condition may become very serious if not treated in time.
- Ultimately patient may go into a coma.
Procedure for ketone bodies:
Gerhardt’s ferric chloride:
- It reacts with acetoacetate only.
- Principle of Gerhardt’s test:
- The reagent is 10% ferric chloride.
- It is based on the reaction of ferric chloride (FeCl3) with acetoacetic acid only, and it will form a red color.
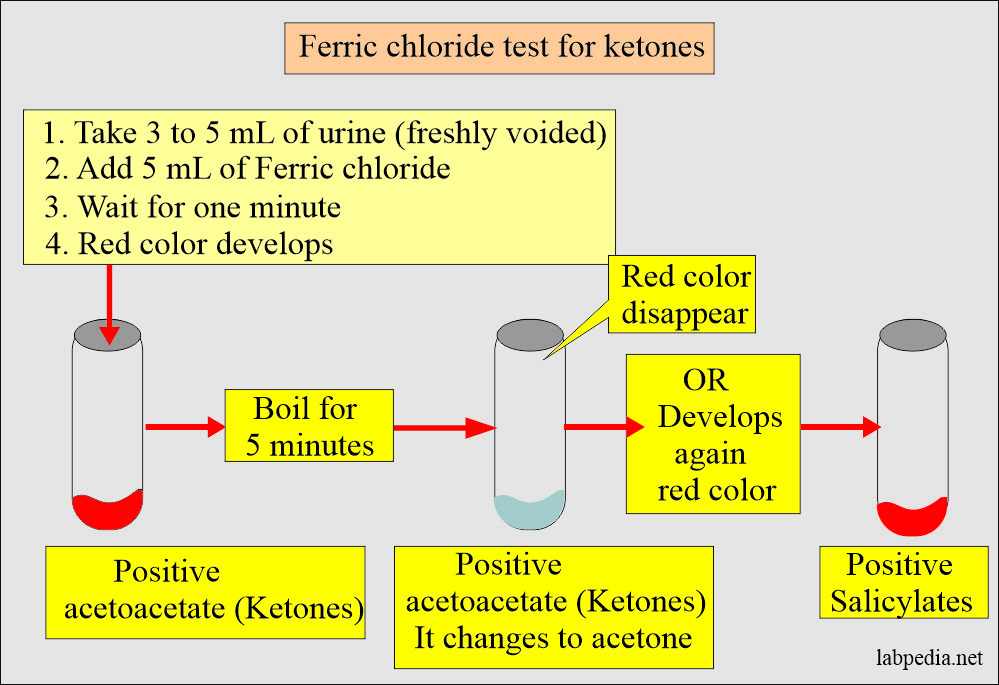
The procedure of Gerhardt’s test:
- Take 3 to 5 mL of urine.
- Add 5 mL of Ferric chloride solution.
- Note the color, if it is red, indicates ketone body, acetoacetic acid.
- Now boil the above solution for 5 minutes.
- Color disappears, indicating acetoacetic acid. By boiling, acetoacetic acid changes to acetone by losing CO2.
- The color remains red, indicating the presence of salicylates.
Nitroprusside Method for ketone bodies:
- It is 10 times more sensitive to acetoacetate than acetone.
Strip method:
- Take urine (freshly voided sample) + add sodium nitroprusside (strips) = Deep violet color in positive cases.
- It has no reaction to β-hydroxybutyrate.
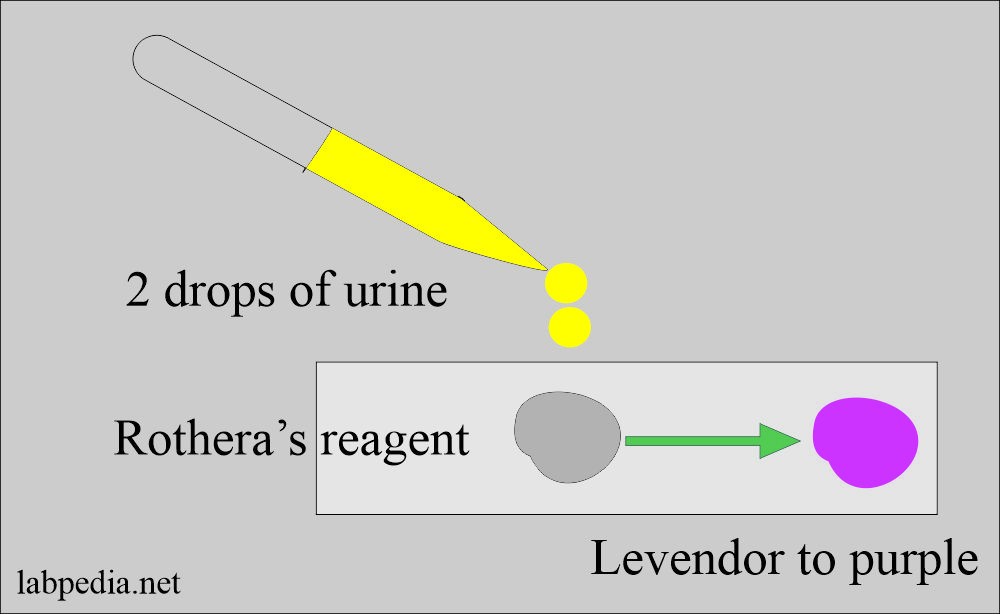
Rothera’s test
- It is the modification of the Nitroprusside method
Nitroprusside tube method:
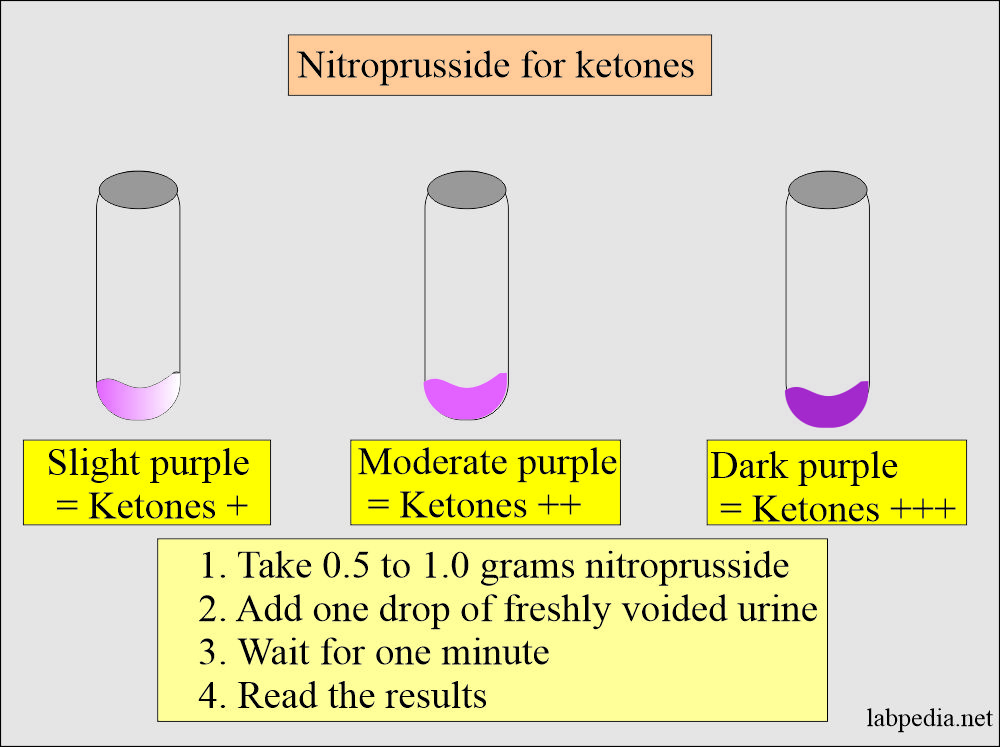
- Add 0.5 to 1.0 grams of nitroprusside to the bottom of the test tube, or can put it on porcelain tile.
- Add one drop of freshly voided urine. Sufficient to moisten the powder.
- Observe for one minute for the development of a mauve-purple color.
- It is easy to assess the color when testing in a test tube. Can see better against the white background.
Results are reported as follows:
| Color change of the reagent | Test result for ketones |
| No color change | Ketones Negative |
| Slight purple color | Ketones are + |
| Moderate purple color | Ketones are ++ |
| Dark purple color | Ketones are +++ |
- For β-hydroxybutyrate, urine is heated to convert β-hydroxybutyrate to acetone and acetoacetate by oxidation.
- Commercial kits are available to estimate the β-hydroxybutyrate.
- Ketone bodies in the urine:
- The urine ketone bodies test detects acetoacetate and acetone.
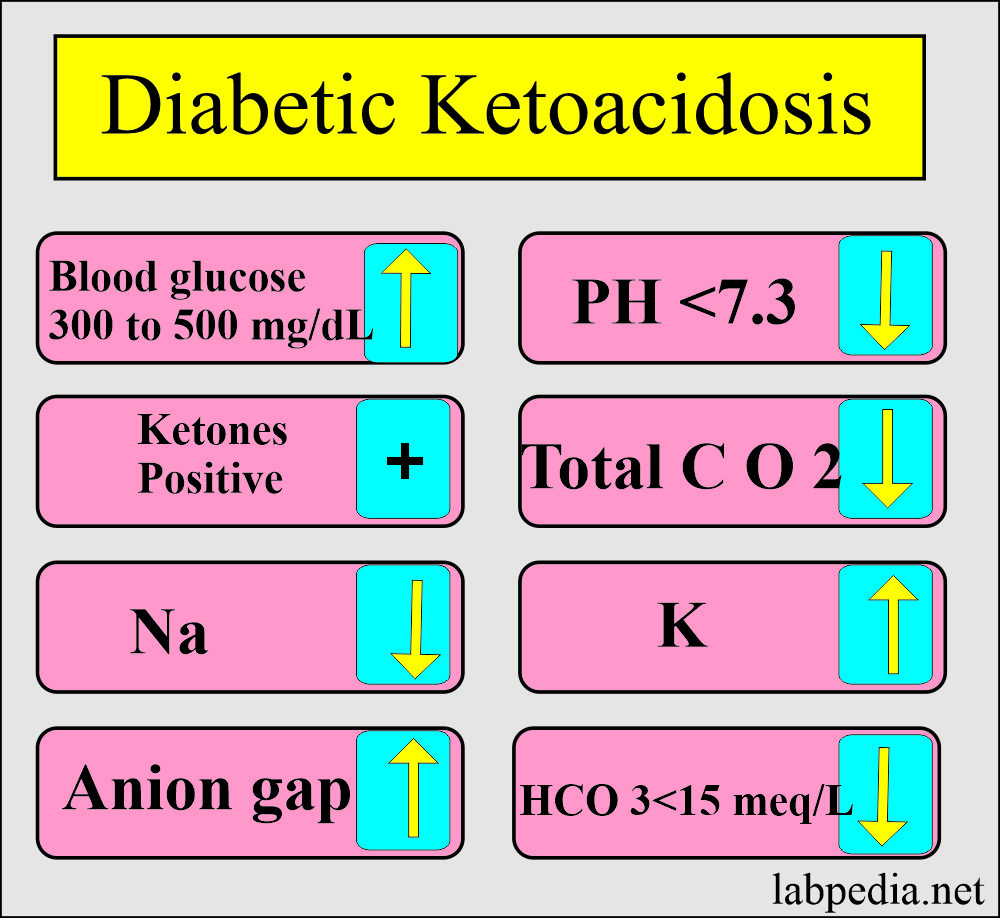
What are the findings in diabetic ketoacidosis?
| Lab test | Result |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
|
What are the complications of diabetic ketoacidosis?
- There is brain edema due to fluid accumulation.
- The patient may have a cardiac arrest.
- The patient may go into kidney failure.
How will you treat diabetic ketoacidosis?
- Start with saline for volume replacement.
- Insulin infusion (but delay if serum potassium level is low <_3.3 meq/L.
- Potassium replacement when the serum level is <5.5 meq/L.
- Glucose drip (5% dextrose with 0.45% saline when the plasma glucose level is <250 mg/dL).
- Continue glucose and insulin until the anion gap is <12 meq/L.
Questions and answers:
Question 1: What is Gerhardt's test?
Question 2: What are complications of diabetic ketoacidosis?
Question 3: What ketone bodies are detected in the urine?