Anemia:- Part 5 A – Sickle Cell Anemia, Discussion and Workup
Sickle Cell Anemia
Sample for Sickle Cell Anemia
- Take EDTA blood for the sickling test.
- Make a fresh smear of the blood.
- Take blood samples for electrophoresis.
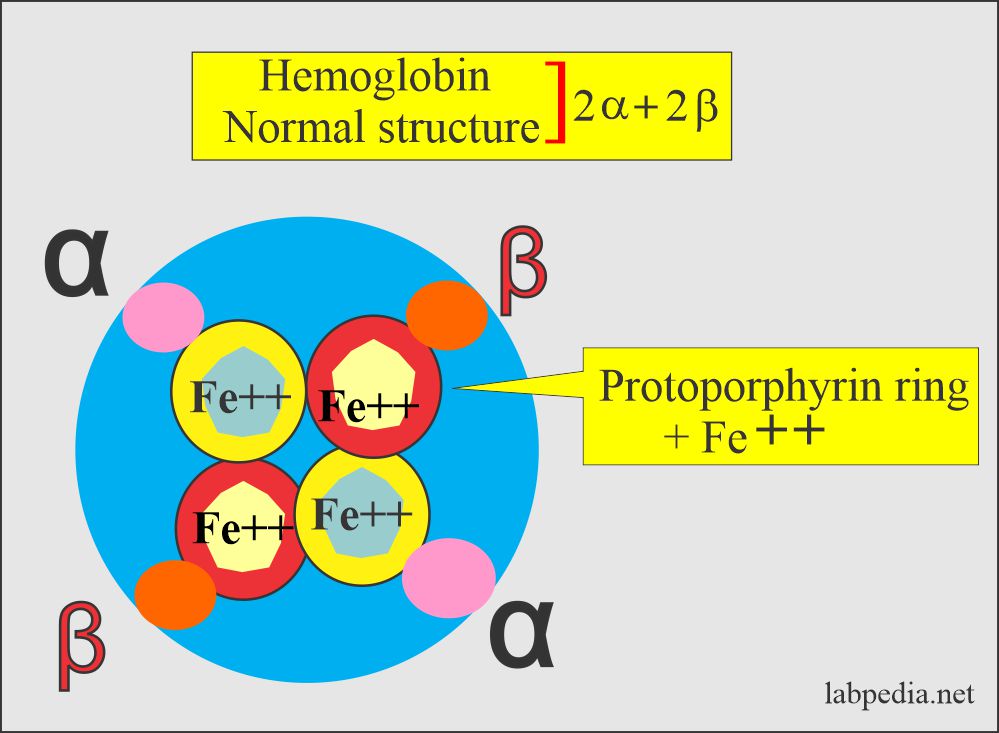
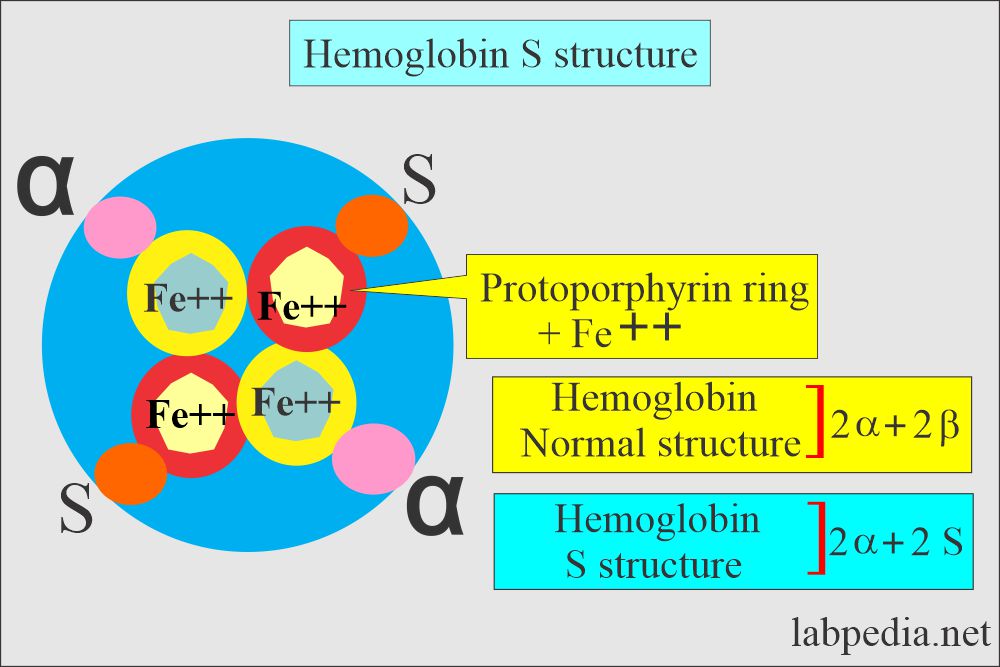
To understand Sickle cell anemia, we need to discuss and understand the structure of the Hemoglobin:
- The normal globin, which is part of the hemoglobin, consists of 2 alpha chains and 2 beta chains.
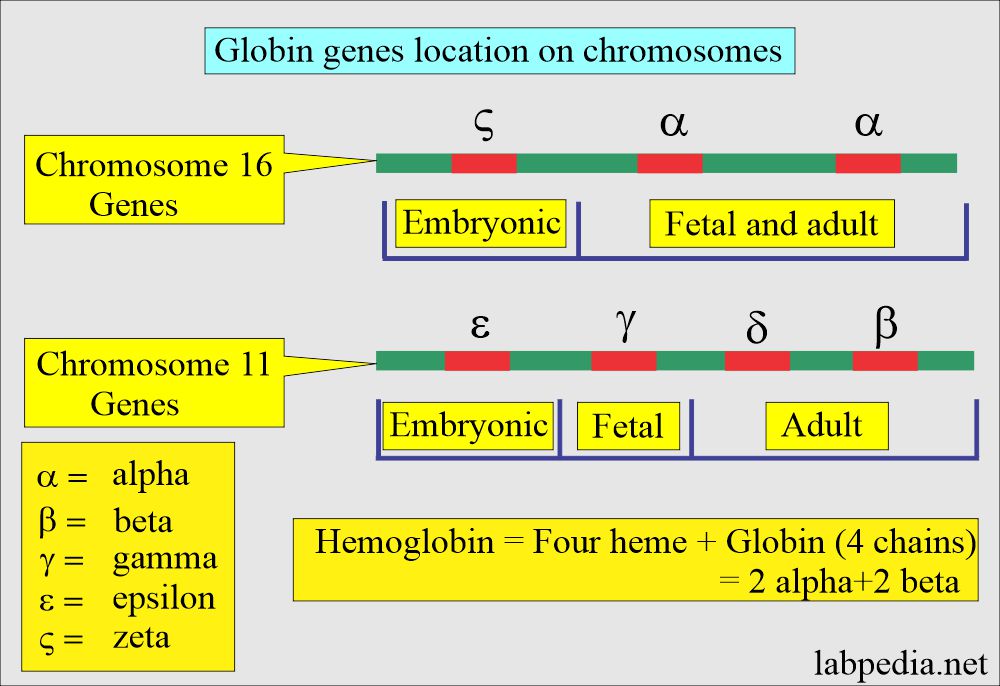
- Genetic code is located on chromosome 11, which are γ, δ, ε, and β-chains.
- While on chromosome 16, there are α and ζ loci.
Various types of hemoglobin:
| Type of hemoglobin | Genotype of hemoglobin | Functions of the hemoglobin |
| Hb A | α2β2 | This is the main adult Hb |
| Hb A2 | α2/δ2 | This is present in a small amount |
| Hb F | α2/γ2 | Main fetal Hb in late stages |
| Hb gower1 | ζ2/ε2 | This Hb is present in the early life of the fetus |
| Hb gower2 | α2/ε2 | This Hb is present in a small amount in the early fetal life |
| Hb portland | ζ2γ2 | This is found in the embryos |
| Hb H | β4 | It is seen in the α-thalassemia |
| Hb Bart’s | γ4 | It is seen in the α-thalassemia |
Sickle cell syndrome:
Background of the sickle cell disease:
- This condition was described in 1910 in Chicag0 in black patients.
- The carrier state in the USA is around 8%, while it is very high in blacks.
- This is also found in Mediterranean countries like Greece, Italy, Israel, Saudi Arabia, India, and Pakistan.
- The sickle gene has some advantages and protects from malarial infection (Plasmodium falciparum).
Definition of Sickle cell disease:
- Sickle cell disease occurs with the autosomal recessive inheritance of abnormal β-chain of the hemoglobin, where glutamic acid is replaced by valine. The end result is precipitation and polymerization of the Hb-S under the conditions of deoxygenation and hypertonicity.
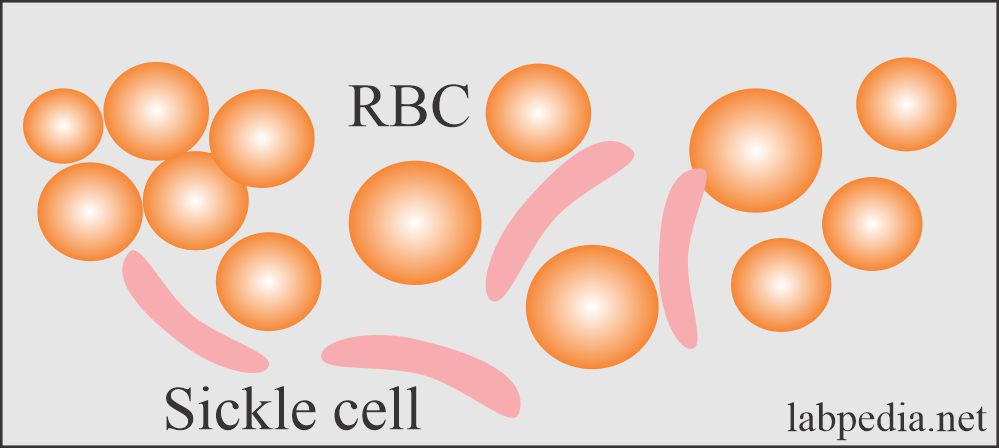
- There is a rigid crystal formation that will deform the RBCs called sickling, and this will lead to the occlusion of the microvasculature and hemolysis.
- Sickle cell disease is defined as where HbA is absent, and only HbS is found. There is a homozygous expression of the S hemoglobin.
Definition of sickle cell anemia:
- In sickle cell anemia. Hemoglobin S agglutinates with deoxygenation and hypertonicity.
- In the case of homozygous disease (HbSS), sickling can occur at physiologic oxygen tension.
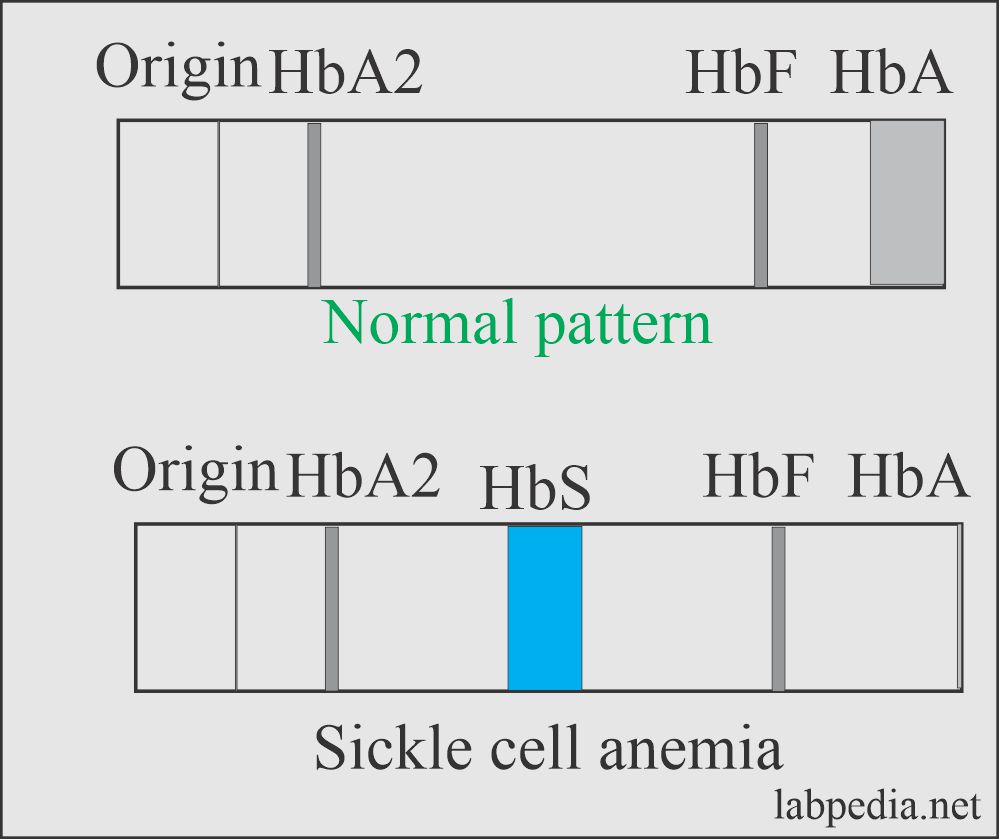
- On electrophoresis, Hb S is 80% to 100%. HbF is the rest, and there is no HbA.
Sickle cell disease:
- It includes all the hemoglobinopathies where HbS is present, e.g.:
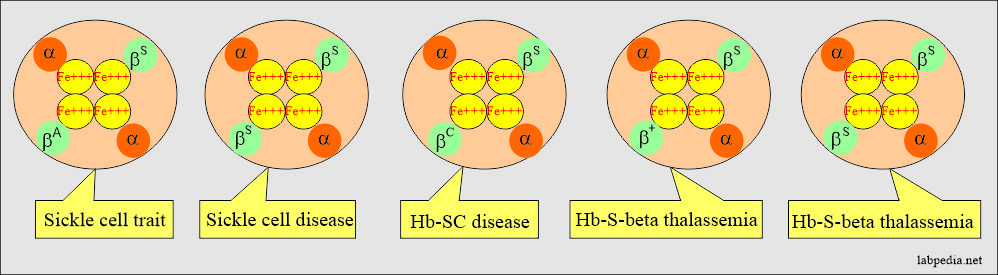
- Sickle cell trait: AS heterozygous (a combination of HbA+HbS = α2 βAβS).
- Hb A = ≅ 60% Hb S = 40%
- Sickle cell disease: SS homozygous (a combination of HbS+HbS = α2 βS βS).
- No HbA, Hb S = >80 Hb F = <1 to 20% Hb A2 = 1% to 4%.
- HbSC disease = α2 βS βC.
- HbS-beta thalassemia disease = α2 βS β0.
- HbS- beta thalassemia = α2 βS β+.
- Sickle cell trait: AS heterozygous (a combination of HbA+HbS = α2 βAβS).
The basic defect in Sickle cell anemia:
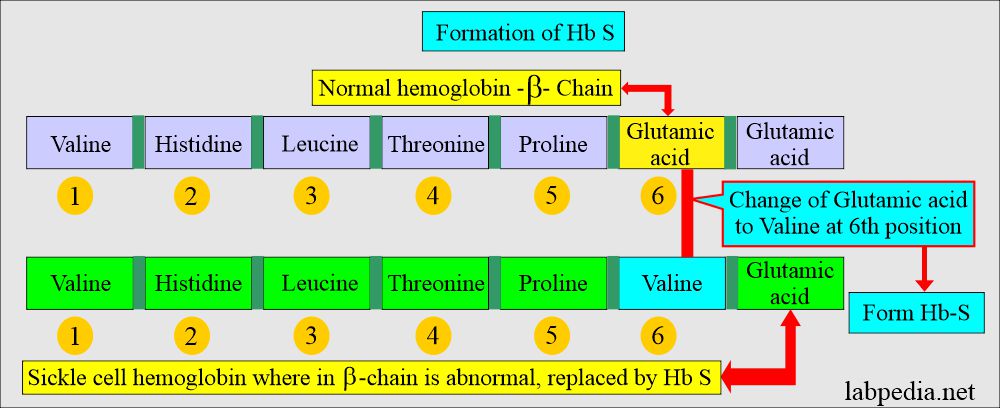
- The amino acid defect is in the β-chain at the 6th position, where the valine replaces the glutamic acid, giving the Hb a lower negative charge than HbA.
- This is the genetic mutation of Glutamic acid to valine.
- Sickle cell RBCs have been transformed into rigid, inflexible cells with at least one prominent projection.
Sickle cell trait (A/S):
- This is a benign condition with no anemia and a normal RBC appearance on the blood smear.
- Hematuria is a common symptom and is thought to be due to small interactions in the kidneys.
- Sickle cell traits are usually asymptomatic.
- This is a heterozygous condition Hb S (α2/β+βS).
- The peripheral blood smear shows normal CBC or mild normocytic or normochromic anemia.
- These patients are at risk of splenic infarcts at high altitudes.
- These patients also have the risk of renal medullary carcinoma.
- Peripheral blood smears also do not show sickle cells.
- Avoid or take care of anesthesia: pregnancy and high altitude.
- Electrophoresis shows:
- Hb S = 35% to 45%,
- Hb F = <1%
- Hb A2 = 1% to 3%
- Hb A = 50% to 55%.
Sickle cells disease (S/S):
- This is a homozygous condition for Hb S (α2/2βS) disease.
- These patients have moderate to severe normochromic and normocytic anemia, and hemoglobin is 5 to 11 g/dL.
- Circulating nucleated RBCs are seen.
- Due to splenectomy, peripheral blood smear may show Howell-Jolly bodies, and anisopoikilocytosis are present because of repeated spleen infarction (autosplenectomy).
- Indirect bilirubin is raised.
- Sickle cell preparation is positive.
- Electrophoresis shows:
- Hb S = >80%
- Hb F = <20%
- Hb A2 = 3% to 8%
- Hb A = absent
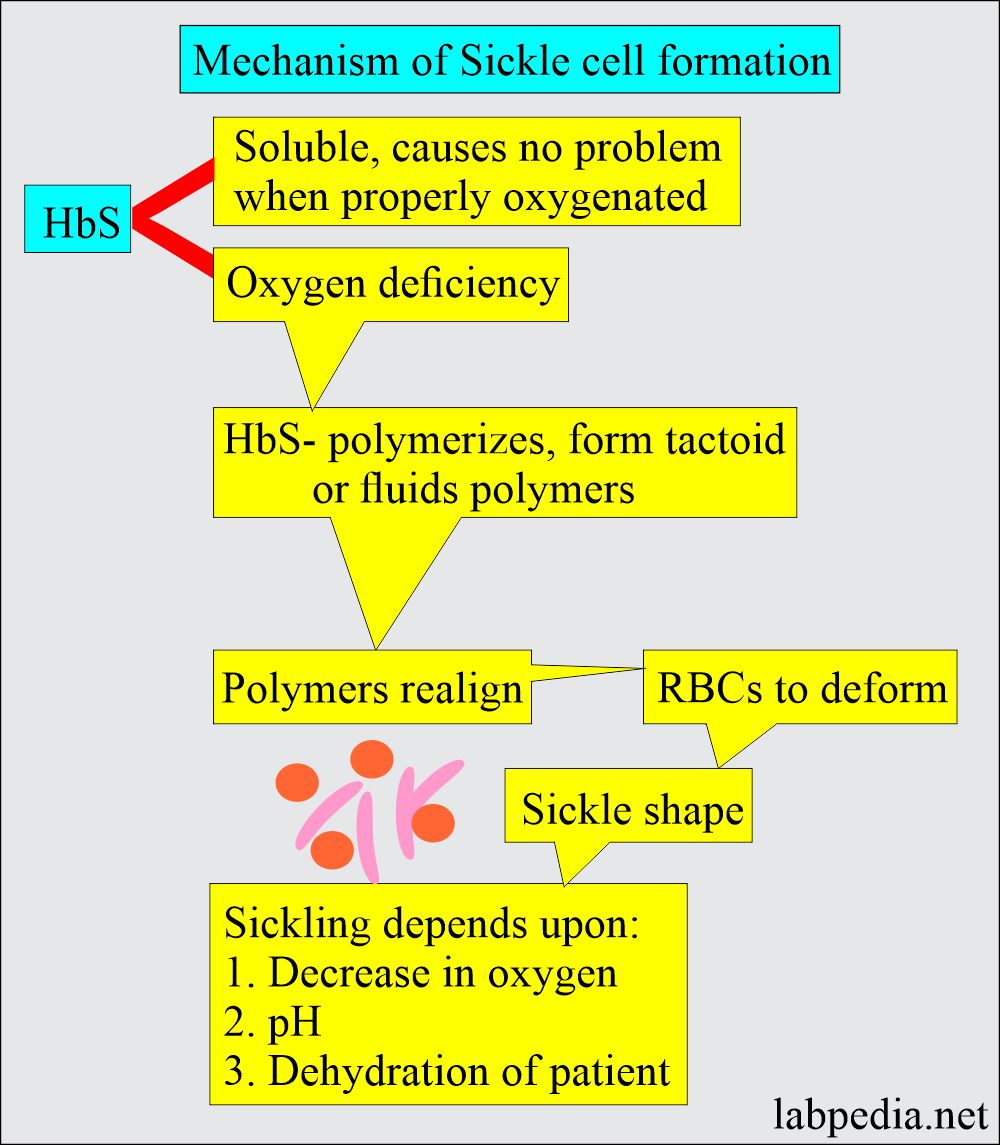
Pathophysiology of Sickling (a mechanism):
- Hb S is soluble and usually causes no problems when properly oxygenated.
- So sickling depends upon the degree of oxygenation.
- When the HbS is deoxygenated in vitro under near physiologic conditions, it becomes relatively insoluble compared to HbA and aggregates into long rigid polymers called tactoids.
- Hb S, called sickle hemoglobin, reacts to deoxygenation and dehydration by solidifying and stretching the RBCs into an elongated sickle -shape, producing hemolytic anemia.
- These sickled RBCs settle in the small blood vessels, giving vaso-occlusive crises, such as abdominal crises, painful crises, and stroke.
- These cells have shortened life in RBCs’ blood by an average of 17 days, whereas the normal half-life of RBCs is 120 days.
- These cells appear crescent in shape on stained blood film.
- These cells return to normal shape when they are oxygenated.
- After several sickling episodes, irreversible damage occurs to these RBCs; these RBCs will be phagocytosed by the macrophagic cells in the liver, spleen, or bone marrow, leading to anemia.
- This process of phagocytosis and hemolytic crises will depend upon the number of damaged RBCs in circulation.
- The rigid sickle RBCs cannot deform and circulate through the small capillaries, resulting in these capillaries’ blockage.
- This will lead to hypoxia and extreme pain and ultimately cause the death of the affected tissue. Infarction in the spleen is common.
- In this case, repeating this process in the spleen will lead to necrosis and scarring, and the result is a nonfunctional spleen called autosplenectomy.
Clinical findings of sickle cell anemia:
- Clinical manifestation of sickle disease does not occur until the infant is 6 months of age. Now decrease in Hb F occurs, and Hb S rises.
- When sickling takes place, which leads to hemolytic anemia, the patient will have the following:
- Pallor and fatigue.
- Jaundice.
- Irritability.
- In the case of acute crises, the patient will manifest a sickle crisis.
Sickle cell crises are:
| Organs involved | Clinical manifestations |
|
|
|
|
|
|
|
|
|
|
|
|
|
|
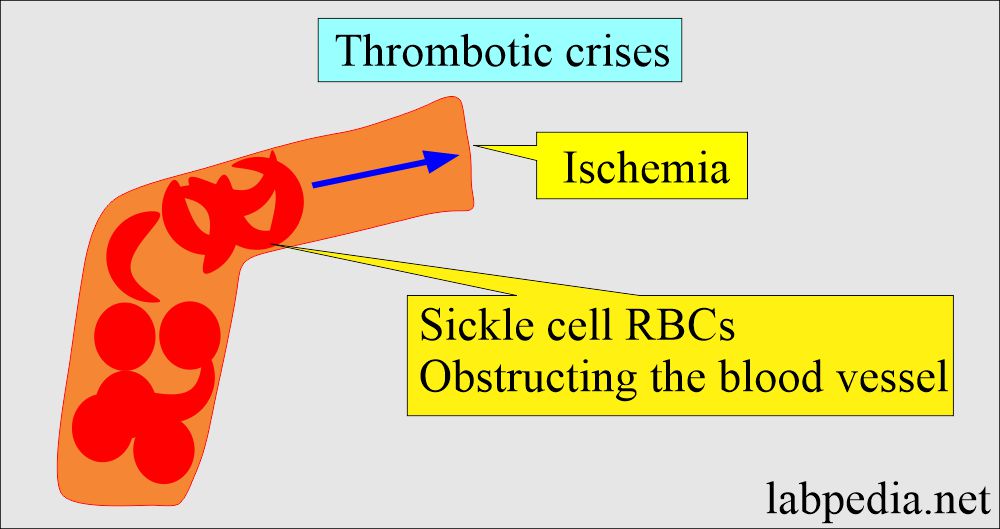
Thrombotic crises (vasoactive changes):
- This will take place due to obstruction of the microcirculation by sickled cells. There are thrombosis and infarction. Vasoactive crises are very painful and may last for days or weeks, with an average duration of 4 to 6 days.
Aplastic crises:
- These are due to decreased erythropoiesis instead of increased need because of hemolytic anemia. This is due to the short life of RBCs, which is just 10 to 20 days. Normally there is compensatory erythropoiesis, 5 to 8 times normal. When this compensatory mechanism is compromised, aplastic crises develop.
Pooling crises:
- These are due to a large pool of blood in the liver and spleen. This type of crisis is seen only in early life. The spleen can hold 1/5th of the body’s blood. There may be death due to cardiovascular collapse.
Hemolytic crises:
- These are unusual but may occur with some drugs or infections.
Infections:
- It is the most common cause of death. Sepsis and meningitis develop in as many as 10% of children during the first 5 years of life and a mortality rate of 25%.
- Survival is unpredictable, but many patients die in their twenties.
Summary of Sickle cell anemia signs and symptoms:
- Anemia.
- Skin manifestations like leg ulcers.
- Arthritis.
- Renal diseases.
- Eye involvement.
- Bone marrow infarcts.
- Autosplenectomy.
- Hepatomegaly.
- Gall bladder stones.
- Priapism.
- GI tract symptoms.
Long-term complications of sickle cells:
- There is an increased susceptibility to infection.
- The spleen may be completely infarcted.
- There are chronic leg ulcers.
- There are gallstones due to repeated hemolysis.
- There may be aseptic necrosis of the bone, particularly femoral heads.
- Chronic renal disease.
- There may be blindness due to retinal detachment or proliferative retinopathy.
- There may be an infarction of the lungs.
- Bone marrow necrosis may cause the fat-emboli syndrome.
Factors influencing the severity of Sickle cell anemia:
It depends upon various factors like:
- Amount of the Hb-S.
- Its association with thalassemia.
- Influence of deoxygenation.
- Presence of amount of Hb-F.
- If it is associated with G6PD deficiency.
- There is the effect of the temperature.
- There is the effect of dehydration.
- It depends upon MCHC.
- Vascular stasis also influences sickle cell disease.
- There is a role in the pH of the body.
Lab findings are of sickle cell anemia:
- Low hemoglobin (7 to 9 G/dL).
- The peripheral blood smear shows sickled RBCs.
- Sickle cell preparation is positive.
- Procedure No 1:
- Take one drop of blood on the slide.
- Put the cover glass and seal the edges with paraffin.
- Characteristic sickling may be seen in 6 hours or earlier.
- This may not be seen after 24 hours.
- Procedure No 2:
- Add reducing substance sodium metabisulfite 2%.
- Metabisulfite is mixed with the blood.
- After mixing with the blood, cover it with cover glass.
- Now seal the edges with paraffin.
- The result may be readable in 15 to 60 minutes.
- Procedure No 3:
- There are commercially available kits based on immunoassays.
- There are antibodies specific for the Hb-S.
- This method is very sensitive for newborn screening.
- This method has no interference by the Hb-F or Hct.
- Procedure No 1:
- Peripheral blood smears show:
- There are marked poikilocytosis and inclusion bodies.
- May see sickle cell 6 to 18% on the peripheral blood smear.
- Platelets are increased.
- Reticulocytes are 10 to 20%.
- ESR is very low.
- Bone marrow shows marked erythroid hyperplasia.
- Iron stain shows low deposits of iron.
- Bilirubin is increased.
- Serum iron is increased.
- TIBC is normal.
- % saturation is normal.
- RBC survival is decreased.
- Electrophoresis of blood shows Hb S and no normal Hb A.
- This is the definitive method for the diagnosis.
- The parents of sickle cell disease will show features of the sickle cell trait.
Laboratory findings in Sickle cell anemia:
| Type of anemia | Hemoglobin | Hct | Reticulocytes | MCV | Hb electrophoresis | RBC morphology | The severity of the disease |
| Sickle cell trait (α2/β+βs) | Usually normal | Usually normal | Normal | Usually normal |
|
Normal | Mostly asymptomatic |
|
Sickle cell disease (α2/βsβs) |
6 to 9 g/dL | 18 to 30 fl | 4 to 30% | 93 |
|
|
It is moderate to severe |
Treatment of sickle cell anemia:
- Prophylaxis:
- Avoid those factors known to precipitate crises, especially dehydration, anoxia, infections, circulation stasis, and skin surface cooling.
- Folic acid 5 mg once weekly should be given.
- Patients should have good general nutrition and hygiene.
- Sickle cell trait does not affect life unless severe hypoxia is caused by shock, vigorous exercise, high altitude, and anesthesia, leading to vasooclusive episodes.
- Sickle cell disease needs supportive treatment for hemolytic anemia and to avoid crises.
- In the case of crises:
- Treat by rest, warmth, rehydration by oral fluids, or I/V normal saline. Can give 3 L in 24 hours.
- Antibiotics are given in case of infection.
- Analgesic is given in case of need, paracetamol, non-steroidal anti-inflammatory agents, and opiates.
- Blood transfusion is given in case of anemia.
- Stem cell transplantation can cure the disease; many patients are successfully treated.
Questions and answers:
Question 1: How much is Hb S in sickle cell disease?
Question 2: What is the most common complication of sickle cells anemia?