Maternal Alpha-Fetoprotein (AFP), and its Significance
Maternal Alpha-Fetoprotein (AFP)
Sample for maternal alpha-fetoprotein (AFP)
- Pregnant mother serum is needed. It is stable for 24 hours at 2 to 8 °C.
- Take 3 to 5 ml of blood in the disposable syringe.
- Keep the syringe for 15 to 30 minutes, and then centrifuge for 2 to 4 minutes. In this way, you can get a clear serum.
Precaution for Maternal alpha-protein
- Keep serum at 2 to 8 °C if the test is performed within 24 hours; otherwise, freeze it at -20 °C.
Indications for Maternal alpha-protein
- This is an effective screening marker for diagnosing body wall defects in the fetus, like neural tube defect, spina bifida, or anencephaly.
- AFP, on average, 25% to 30%, has a low value in Down’s syndrome.
- This test is indicated in pregnant ladies who have the following findings:
- Female over the age of 35 years.
- If there is a family history of birth defects.
- If the lady has taken harmful medications during pregnancy.
- Female with a history of diabetes mellitus.
Definition of Alpha-fetoprotein (AFP):
- The fetal liver produces α1-globulin called alpha-fetoprotein (AFP).
- AFP will become the dominant fetal protein in the first trimester, reaching its peak at 12 weeks of gestation.
- During the first 10 weeks of fetal life, the major serum protein is not albumin; this is actually alpha-fetoprotein (AFP)
- AFP has the same sequence of amino acids as albumin. Suggesting the same gene ancestor.
- It, later on, declines to 1% at birth.
Molecular structure and development of Alpha-fetoprotein (AFP):
- The fetal liver produces alpha-fetoprotein (AFP), becoming the dominant fetal protein in the first trimester, reaching a peak at 12 weeks of intrauterine fetal life. It declined to 1%of the peak at birth.
- AFP is a glycoprotein first produced by the yolk sac and then by the fetal liver.
- It reaches to peak at 10 to 13 weeks of gestation, later declining to <10 µg/L by the term.
- By the age of 2 years, it reaches the adult level (<5 µg/L)
- AFP (α1- Fetoprotein) has 40% carbohydrates with a molecular mass of 70 kD. This is also called α1- Fetoprotein.
- AFP is a glycoprotein that migrates more slowly on electrophoresis than albumin but is faster-moving than other globulins.
- AFP is an oncofetal protein (glycoprotein) synthesized in the fetal liver and yolk sac.
- AFP is very stable in serum, even at room temperature, for as long as a week.
- The AFP gene is located on the long arm (q) of chromosome 4 (q11 to q22). This is part of the family gene for albumin and vitamin D-binding protein.
- Some of the fetal AFP enters the maternal serum (circulation).
- AFP is the dominant fetal serum protein in the first trimester.
- It is very low at the age of one year.
Maternal Alpha-Fetoprotein (AFP):
- Maternal AFP rises progressively in the first and second trimesters.
- Maternal serum reaches its peak at the 13th week of gestation, then declines rapidly to <2% of the maximum level by 34 to 36 weeks of pregnancy.
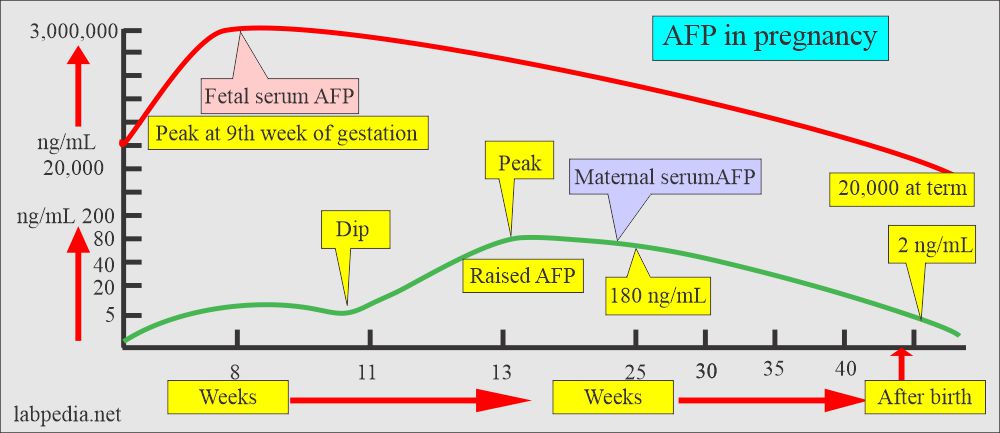
- The AFP at the 8th week is very high; then there is a dip at 11 weeks and again peaks at 13 weeks. Then fall in a long-linear fashion till 25 weeks.
- Maternal AFP is 5 ng/mL at the 10th-week gestation, then increases by 15% per week. The 25th week is 180 ng/mL, then decline slowly until term.
- After birth, it drops to 2 ng/mL.
Fetal AFP pattern:
- In the early stages, AFP is produced in the yolk sac and is small in quantity. The fetal liver produces a major quantity, and the yolk sac degenerates.
- AFP has a high concentration in the fetal serum early in embryonic life.
- The peak concentration is 3,000,000 ng/mL at 9 weeks of gestation. Then concentration declines steadily to 20,000 ng/mL at term.
- In infants, the AFP level declines and reaches the adult level by the 10th month of life.
- By the age of one year, a greater decrease occurred.
Functions of the AFP:
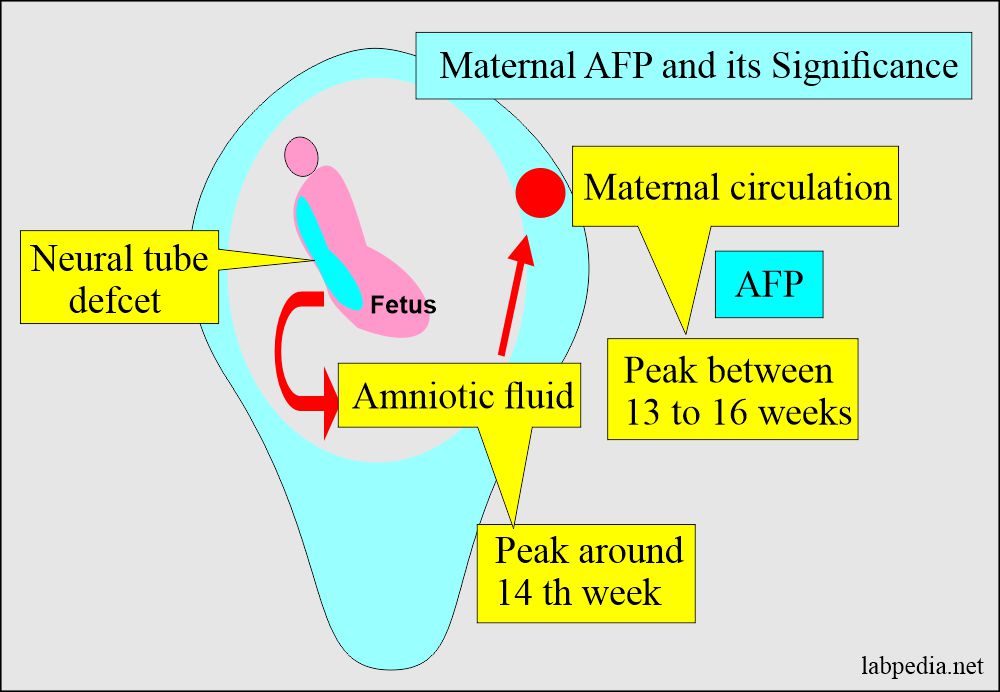
- Amniotic AFP is more accurate in diagnosing neural tube defects in the early gestation (around 14 weeks) than maternal serum AFP.
- Neural tubes defect varies from small myelomeningocele to anencephaly.
- Other fetal body wall defects are:
- Omphalocele.
- Gastroschisis.
- Before 14 weeks, AFP helps to diagnose neural tube defects.
- Normal AFP <2.5 Multiples of median (MoM).
- For the neural tube, the defect is >2.5 MoM.
- If there is a body wall defect in the fetus, AFP leaks out into amniotic fluid and is picked up by the maternal circulation.
- If there is an increased AFP level, then further evaluation by repeated AFP, amniotic fluid AFP, and ultrasound.
- The serum AFP level is 100 times that of amniotic fluid.
- AFP is used to diagnose neural tube defects.
- Raised AFP level may indicate multiple pregnancies, fetal distress, congenital fetal abnormalities, or intrauterine death.
- A Low AFP level may diagnose Down’s syndrome (trisomy 21).
- AFP is used as a tumor marker.
Maternal serum screening of the alpha-fetoprotein (AFP):
- There is the possibility of 3% birth defects in newborns.
- Early detection of the fetus abnormality is the goal of maternal serum AFP estimation.
- In most cases, AFP estimation is recommended during 16 to 18 weeks of gestation. The specimen is collected during 14 to 20 weeks of gestation.
- If it is delayed, then deciding to terminate the pregnancy is difficult, like elective termination of pregnancy.
- In the case of neural tube defect, there is increased fetal amniotic fluid and mother serum AFP.
- Maternal serum AFP helped diagnose open neural tube defects.
- 90% of newborns with neural tube defect has no known risk factors.
- In down’s syndrome, the maternal serum AFP is low.
- Tripple screening test done in the second trimester to find potential birth defect includes:
- Maternal Serum AFP.
- Maternal HCG.
- Maternal Estriol level.
Normal values of AFP
| Maternal serum level AFP | |
| 14 weeks of gestation | 25.6 ng/mL (median) |
| 16 weeks of gestation | 34.8 ng/mL (median) |
| 18 weeks of gestation | 47.3 ng/mL (median) |
| 20 weeks of gestation | 64.3 ng/mL (median) |
| 21 weeks of gestation | 74.9 ng/mL (median) |
| Fetal serum level AFP | |
| First-trimester peak |
|
| Cord blood | <5 mg/dL |
| Adult AFP | |
| 97% of the healthy population | <8.5 ng/dL |
| 100% of the healthy population | <15.0 ng/dL |
Source 2
- Adult = <40 ng/mL (<40 mcg/L)
- Child (<1 year) = <30 ng/mL
Another source
- 25 ng/mL (25 µg/L).
- At 15 to 18 weeks of gestation = 10 to 150 ng/mL (10 to 150 µg/L).
Raised AFP level seen in:
- Maternal serum level >2 times the median level will be seen in:
- Multiple gestations (multiple pregnancies).
- Fetal death.
- Malformations, e.g., open neural tubes defects like anencephaly, open spinal Bifida, encephalocele, and myelocele.
- 80% of the cases are diagnosed by AFP level (hydrocephaly and microcephaly).
- Maternal serum and amniotic fluid Increased AFP concentration:
- Open neural tube defects like anencephaly, spina bifida, omphalocele, esophageal or duodenal atresia.
- Threatened abortion.
- Fetal distress.
- Intrauterine death of the fetus.
- Fetal congenital abnormalities.
- Abdominal wall defects like gastroschisis.
- Other conditions for raised AFP are:
- Renal abnormalities
- Cystic hygroma.
- Hydrops fetalis.
- Turner syndrome.
- Bowel obstruction.
- Twins.
- Feto-maternal hemorrhage.
- Sacrococcygeal Teratoma.
- Esophageal or duodenal atresia.
- Renal disorders like polycystic kidney, renal agenesis, and urethral obstruction.
- Tetralogy of Fallot.
- Oligohydramnios.
- Turner syndrome.
- Placental causes like thrombosis, infarction, very large placenta, and cystic changes.
- Maternal causes like tumor-producing AFP and hepatitis.
Decreased Maternal Alpha-Fetoprotein (AFP) is seen in:
- Down syndrome (Trisomy 21).
- Long-standing death of the fetus.
- Molar pregnancy (Hydatidiform mole).
- Choriocarcinoma.
- Spontaneous abortion.
- Overestimated gestational age.
- Pseudopregnancy.
- A low level of AFP with an abnormal value of HCG and estriol (Triple screening) is indicative of :
- Trisomy 21 (Down’s syndrome).
- Trisomy 18 (Edwards syndrome)
- Or other chromosomal abnormalities.
- Women with diabetes mellitus have 20% to 40% lower values than nondiabetic women.
Increased maternal AFP is seen in (Also do amniotic fluid AFP):
- Multiple pregnancies.
- Open neural tube defects like:
- Open spina bifida.
- Encephalocele.
- Myelocele.
- Anencephaly.
- Sacrococcygeal teratoma.
- Turner syndrome.
- Omphalocele.
- Gastroschisis.
- Hydrops fetalis.
- Intrauterine death.
- Feto-maternal hemorrhage.
- Esophageal or duodenal atresia.
- Tetralogy of Fallot.
- Oligohydramnios.
- Cystic hygroma.
- Placental causes are:
- Thrombosis.
- Infarction.
- Cystic changes.
- Infections.
- Very large placenta.
- Rarely benign hereditary familial raised level of AFP.
- Maternal causes:
- Hepatitis.
- Malignancies producing AFP.
Markers to detect fetal abnormalities:
| Clinical presentation | Maternal AFP | Maternal HCG | Estriol (unconjugated) | The success rate of detection |
| Open spina bifida | Increased (+++) | Negative | Negative | 80% |
| Anencephaly | Increased (++++) | Negative | Negative | 95% |
| Abdominal wall defect | Increased (+++) | Negative | Negative | 75% |
| Down’s syndrome (Trisomy 21) | Decreased | Increased | Decreased | 60% |
| Trisomy 18 | Markedly decreased | Markedly decreased | Markedly decreased | 60% |
Questions and answers:
Question 1: What is the significance of maternal alpha-fetoprotein?
Question 2: What is the value of maternal AFP when the value is high?
Question 3: When AFP is low and why?